Hip Fractures:
Symptoms, Causes and Treatments






A hip fracture can happen in an instant, whether from a simple fall at home or a sudden loss of balance. For many people, especially older adults, it can be a frightening and painful experience that immediately affects mobility and independence.
Because the hip plays a central role in standing, walking and sitting, even small movements can become extremely uncomfortable after a fracture. While some stable fractures may be managed carefully without surgery, many require timely surgical treatment to restore movement and reduce the risk of complications. With appropriate care and rehabilitation, recovery is possible and many patients are able to regain their function and quality of life.
What Are the Common Symptoms of Hip Fractures?
Symptoms of a hip fracture may appear suddenly after a fall or develop over time in stress fractures, but recognising them early helps prevent worsening complications. Common signs include:
Severe Hip Pain
Pain typically occurs immediately after a fall or injury and is concentrated in the groin, outer hip, or upper thigh. This pain is sharp with movement, making it difficult to bear weight or walk.
Inability to Bear Weight
Most patients cannot put weight on the affected leg, which makes standing, walking, or even shifting in bed extremely difficult and unsafe.
Leg Shortening or Rotation
The injured leg may appear shorter or externally rotated due to displacement of the femoral head, which is a clear visual indicator of a hip fracture.
Swelling or Bruising
Soft tissue around the hip may swell or bruise quickly, signalling trauma to the bone and surrounding tissues and helping differentiate fractures from muscle strains.
Difficulty Moving the Hip
Even small movements, like bending the hip or lifting the leg, trigger sharp pain or instability, indicating structural disruption in the hip joint.
Why It Happens
What Causes Hip Fractures?
Hip fractures usually occur when significant force is applied to the upper part of the thigh bone near the hip joint. In older adults, this force is often the result of a fall. In younger individuals, it may be due to high-impact trauma or repetitive stress.
Falls
Falls are the most common cause of hip fractures, particularly among older adults. The impact of landing on the side of the hip places sudden force on the femur, which can lead to a break, especially if the bone is already weakened.
High-Impact Trauma
Car accidents, sports injuries or other high-energy impacts can cause hip fractures even in otherwise healthy bones. These injuries are often more severe and may require surgical repair.
Stress Fractures
Less commonly, small cracks can develop in the femoral neck due to repetitive strain, particularly in athletes, military recruits or individuals with reduced bone strength. Without rest and treatment, these stress fractures may progress to a complete break.
Know Your Risk Profile
What Are the Risk Factors for Hip Fractures?
While a fall or trauma may trigger the fracture, certain factors increase the likelihood that the bone will break when force is applied. These risk factors either weaken the bone itself or raise the chances of falling.
Ageing
Bone density naturally decreases with age, making bones more fragile. At the same time, balance and reaction time may decline, increasing the risk of falls.
Osteoporosis or Bone Conditions
Osteoporosis reduces bone mass and weakens bone structure, making the femur more susceptible to fracture even from minor trauma. Other metabolic bone disorders can have a similar effect.
Post-Menopausal Changes
After menopause, lower oestrogen levels accelerate bone loss. This makes women particularly vulnerable to osteoporosis and hip fractures.
Previous Falls or Injuries
A history of falls or prior fractures may indicate underlying balance issues, reduced bone strength or both, increasing the likelihood of future injury.
Physical Inactivity
Weak muscles, reduced coordination and poor balance can increase the risk of falling. Regular weight-bearing activity helps maintain bone strength and stability.
Medications or Chronic Conditions
Certain medications may affect bone density, balance or alertness. Chronic illnesses, neurological conditions or visual impairment can also increase the likelihood of falls and subsequent fractures.
Vision or Balance Impairments
Impaired vision, vestibular issues or neurological problems can cause missteps or falls, directly contributing to fracture occurrence.
Understanding the Differences
Types of Hip Fractures
Hip fractures are classified based on where the break occurs along the upper femur and whether the bone has shifted from its normal position. Knowing the type helps your orthopaedic specialist predict recovery, as each fracture location affects blood supply, stability and hip movement differently.
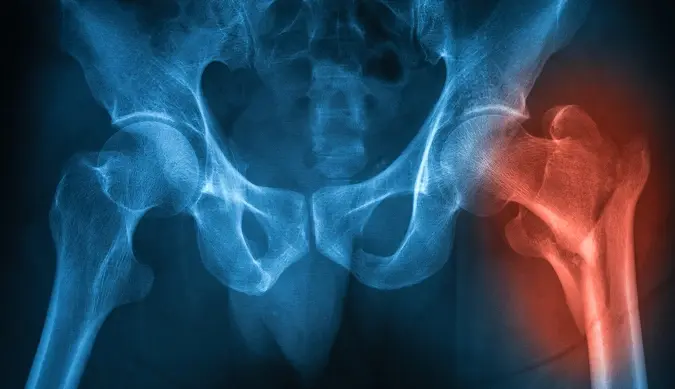
Femoral Neck Fracture
This fracture happens just below the ball of the hip joint, disrupting blood flow to the femoral head, increasing the risk of complications and often requires surgery to restore stability and prevent long-term problems.
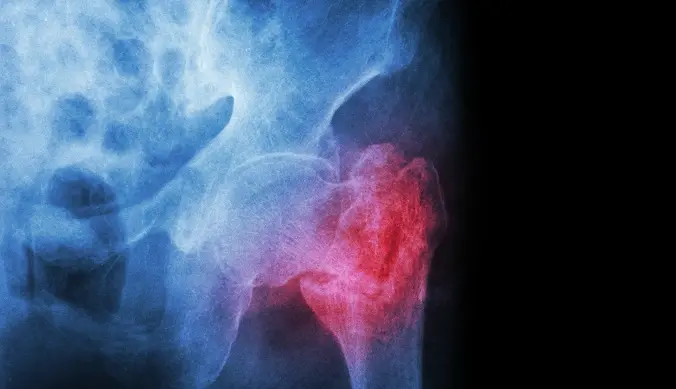
Intertrochanteric Fracture
Located further down the femur, this fracture usually results from a fall. Surgery with plates or screws is commonly needed to hold the bone in place and allow the hip to heal safely.
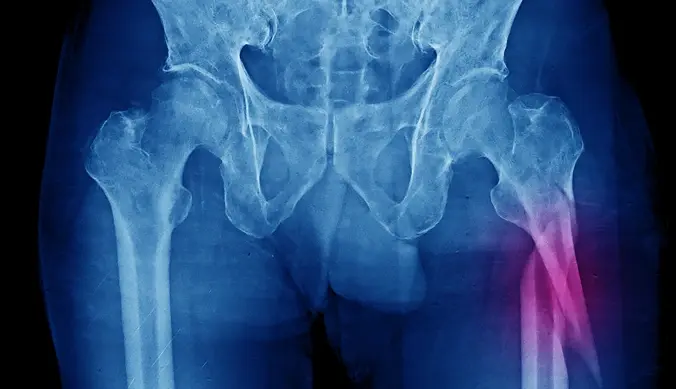
Subtrochanteric Fracture
Found below the intertrochanteric area along the upper femur shaft, these fractures often occur from high-energy trauma. Complex surgical repair is usually necessary to restore hip stability, strength and mobility during recovery.
Understanding Your Evaluation
How Are Hip Fractures Diagnosed?
While many hip fractures cause obvious pain and difficulty bearing weight, some non-displaced or stress fractures can present with symptoms similar to arthritis or soft tissue injuries. Accurate diagnosis is, therefore, essential. Your orthopaedic specialist will confirm whether a fracture is present, determine its type and severity and evaluate surrounding tissues for complications.
Understanding Your Evaluation
How Are Hip Fractures Diagnosed?
While many hip fractures cause obvious pain and difficulty bearing weight, some non-displaced or stress fractures can present with symptoms similar to arthritis or soft tissue injuries. Accurate diagnosis is, therefore, essential. Your orthopaedic specialist will confirm whether a fracture is present, determine its type and severity and evaluate surrounding tissues for complications.
Physical Examination
Your orthopaedic specialist will assess your ability to move the leg and bear weight. They will look for signs such as leg shortening, outward rotation, swelling and tenderness around the hip. Pain triggered by gentle movement of the hip can help localise the source of injury and raise suspicion of a fracture.
X-ray
X-rays are typically the first-line imaging test for suspected hip fractures. They can confirm most fractures, show whether the bone has shifted from its normal position and provide information about overall bone quality.
CT Scan or MRI
If the fracture is complex or not clearly visible on X-ray, further imaging may be required. CT scans provide detailed views of the bone structure and are useful for assessing complicated fracture patterns. MRI is particularly valuable when an X-ray appears normal but a fracture is still suspected, as it can detect subtle or occult fractures and assess surrounding soft tissues.
Hip Fractures Treatments in Singapore
Hip fracture treatments in Singapore usually depend on the fracture type, degree of displacement, bone quality, age and overall health of the patient. The primary goals are to relieve pain, restore mobility, promote safe healing and reduce the risk of complications such as blood clots, muscle loss or prolonged immobility.
Non-surgical Management
Non-surgical care is generally reserved for stable, non-displaced fractures or for patients who are medically unfit for surgery. This approach may involve protected weight-bearing, pain control and close monitoring with follow-up imaging. Physiotherapy is introduced early to maintain muscle strength and reduce complications associated with prolonged bed rest.
Internal Fixation Surgery
Internal fixation is commonly used for stable or certain displaced fractures where preserving the natural hip joint is appropriate. Metal screws, plates or an intramedullary nail are inserted to stabilise the broken bone and hold it in proper alignment during healing. This method allows earlier mobilisation and helps maintain the patient’s native hip joint, particularly in younger individuals or selected fracture patterns.
Partial Hip Replacement
Partial hip replacement, also known as hemiarthroplasty, involves replacing the fractured femoral head while leaving the natural hip socket intact. It is frequently recommended for displaced femoral neck fractures, especially in older adults. This procedure reduces the risk of complications associated with disrupted blood supply to the femoral head and allows safer and earlier mobilisation after surgery.
Total Hip Replacement
Total hip replacement may be considered for severe fractures, fractures involving joint damage or patients with pre-existing hip arthritis. Both the femoral head and the hip socket are replaced with prosthetic components. This procedure can provide better long-term function and pain relief in appropriately selected patients, especially those who were independently mobile before the injury.
Rehabilitation and Recovery
Early rehabilitation is essential regardless of the treatment approach. Guided physiotherapy focuses on restoring strength, balance and walking ability. A structured rehabilitation plan helps reduce the risk of future falls and supports a safe return to daily activities.
Personalised Hip Fracture Care at HC Orthopaedic Surgery
A hip fracture demands timely surgical decision-making, precise stabilisation and structured rehabilitation to prevent long-term disability. Without appropriate treatment, complications such as muscle loss, blood clots and prolonged immobility can significantly affect recovery. Early intervention not only repairs the fracture but also supports safe mobilisation, restores confidence in movement and reduces the risk of future falls through proper bone health optimisation.

Personalised Hip Fracture Care at HC Orthopaedic Surgery
A hip fracture demands timely surgical decision-making, precise stabilisation and structured rehabilitation to prevent long-term disability. Without appropriate treatment, complications such as muscle loss, blood clots and prolonged immobility can significantly affect recovery. Early intervention not only repairs the fracture but also supports safe mobilisation, restores confidence in movement and reduces the risk of future falls through proper bone health optimisation.
Our Specialised Team
At HC Orthopaedic Surgery, hip fracture care is led by Dr Henry Chan, together with Dr Nicholas Yeoh, Dr Toon Dong Hao and Dr Tang Zhi Hao. Dr Chan has a special interest in computer-assisted joint replacement surgery and previously spearheaded the Joint Replacement Unit at Tan Tock Seng Hospital, where he performed more than 1,000 joint replacements. In addition, Dr Yeoh completed advanced fellowship training in hip and knee reconstruction at the internationally recognised, high-volume North Sydney Orthopaedic and Sports Medicine Centre, Mater Hospital, Sydney. Together, the team provides comprehensive assessment and tailored treatment to help patients recover safely and return to daily life with confidence.
Frequently Asked Questions (FAQs) About Hip Fractures
How long does it take to recover from a hip fracture?
How soon should surgery be done after a hip fracture?
What are the risks of hip fracture surgery?
How can I prevent future hip fractures?
Will I walk normally again after a hip fracture?
Can hip fractures lead to long-term complications?
Does osteoporosis increase the risk of hip fractures?
Can I live independently after a hip fracture?
Meet Our Specialist Team
Our team comprises Dr Henry Chan, Dr Nicholas Yeoh, Dr Toon Dong Hao, and Dr Tang Zhi Hao — experienced orthopaedic surgeons with subspecialty experience and a patient-centred approach to care.

Dr Henry Chan
Medical Director & Senior Consultant Orthopaedic Surgeon
MBBS (S’pore), MRCS (Edinburgh), MMed (Orthopaedic Surgery), FRCS (Edinburgh)
Dr Henry Chan is an experienced orthopaedic surgeon specialising in joint replacement and complex revision surgery. Trained at the renowned Helios Endo-Klinik in Germany under the MOH HMDP scholarship, he has performed over 1,000 joint replacements and specialises in computer-assisted and robotic joint replacement techniques for precise outcomes.

Dr Nicholas Yeoh
Senior Consultant Orthopaedic Surgeon
MBChB (Edinburgh), MRCS (Edinburgh), MMed (Orthopaedic Surgery), FRCS (Edinburgh)
Dr Nicholas Yeoh is an MOH-accredited orthopaedic specialist and Fellow of the Royal College of Surgeons of Edinburgh. Fellowship-trained in hip and knee reconstruction in Sydney under the MOH HMDP scholarship, he specialises in minimally invasive joint replacement, robotic surgery and advanced techniques that enhance recovery and surgical outcomes.

Dr Toon Dong Hao
Senior Consultant Orthopaedic Surgeon
MBChB (Leeds), MRCS (Edinburgh), MMed (Orthopaedic Surgery), FRCS (Edinburgh)
Dr Toon Dong Hao is a skilled orthopaedic surgeon and Fellow of the Royal College of Surgeons of Edinburgh. Fellowship-trained in Advanced Shoulder and Elbow Surgery in Sydney under the MOH HMDP scholarship, Dr Toon specialises in sports injuries, arthroscopic surgery and complex shoulder, elbow and knee procedures to restore function and mobility.

Dr Tang Zhi Hao
Senior Consultant Orthopaedic Surgeon
MBBS (S’pore), MRCS (Edinburgh), MMed (Orthopaedic Surgery), FRCS (Edinburgh)
Dr Tang Zhi Hao is a fellowship-trained orthopaedic surgeon specialising in foot and ankle conditions. He completed his Foot and Ankle Surgery fellowship at Severance Hospital, Yonsei University Health System in Seoul under Professor Jin Woo Lee. Prior to private practice, he served as Consultant and Deputy Head of Orthopaedics at Khoo Teck Puat Hospital.