Elderly (Geriatric) Fracture:
Symptoms, Causes and Treatments






Elderly, or geriatric, bone fractures are an increasingly common concern in Singapore’s rapidly ageing population. As more residents live into their 70s and 80s, age-related conditions such as osteopenia and osteoporosis are becoming more prevalent. These conditions weaken the bones, making them more prone to fractures even after a minor fall or simple daily activity.
Unlike younger individuals, older adults often have reduced muscle strength, poorer balance and lower physiological reserves. As a result, fractures of the hip, spine and wrist can occur more easily and may lead to prolonged hospital stays, loss of independence and slower recovery. Geriatric fractures are not just isolated injuries. They often reflect underlying bone fragility and frailty. Effective treatment therefore goes beyond fixing the broken bone. It includes optimising bone health, preventing future falls and supporting rehabilitation, all of which are essential in maintaining quality of life in later years.
What Are the Common Symptoms of Geriatric Fracture?
Symptoms of geriatric fractures cause sudden and obvious pain; others, such as spinal compression fractures, may develop gradually and feel less severe at first.
Common symptoms include:
Sudden Pain
Pain often occurs immediately after a fall or injury. It may feel sharp or deep and typically worsens with movement or pressure over the affected area.
Swelling and Bruising
Swelling, redness or bruising may appear around the injured site. This is more noticeable in fractures involving the wrist, ankle or hip.
Difficulty Moving the Limb
A fracture may make it difficult to move the affected limb normally. Simple actions such as standing, lifting the arm or turning the body may become painful.
Inability to Bear Weight
Many older adults struggle to stand or walk after a fracture, especially with hip or pelvic injuries. The limb may feel weak, unstable or unable to support body weight.
Pain in the Hip, Groin or Thigh
Hip fractures often cause pain in the outer hip, pelvis, groin or upper thigh. The discomfort may also radiate down the leg.
Visible Deformity
Some fractures cause the limb or joint to look out of alignment. In severe cases, one leg may appear shorter or turned outward compared to the other.
Loss of Height or Curved Spine
Spinal compression fractures may lead to a gradual loss of height or a more hunched posture. Some individuals notice worsening back pain and a visible curvature of the upper spine.
Reduced Function and Mobility
Fractures can lead to a sudden decline in independence. Everyday activities such as walking, dressing or getting up from a chair may become difficult without assistance.
Why It Happens
What Causes Fractures in the Elderly?
Fractures occur when a bone is exposed to more force than it can withstand. In older adults, bones are often weaker due to age-related bone loss, which means even minor injuries can lead to fractures. Common causes include:
Falls
Falls are the most frequent cause, often linked to poor balance, muscle weakness, vision problems or home hazards.
Trauma
Although less common than falls, higher-impact injuries such as road traffic accidents can also cause fractures in older individuals.
Know Your Risk Profile
What Are the Risk Factors for Geriatric Fractures?
Certain health and lifestyle factors can increase the risk of fractures in older adults. These include:
Know Your Risk Profile
What Are the Risk Factors for Geriatric Fractures?
Certain health and lifestyle factors can increase the risk of fractures in older adults. These include:
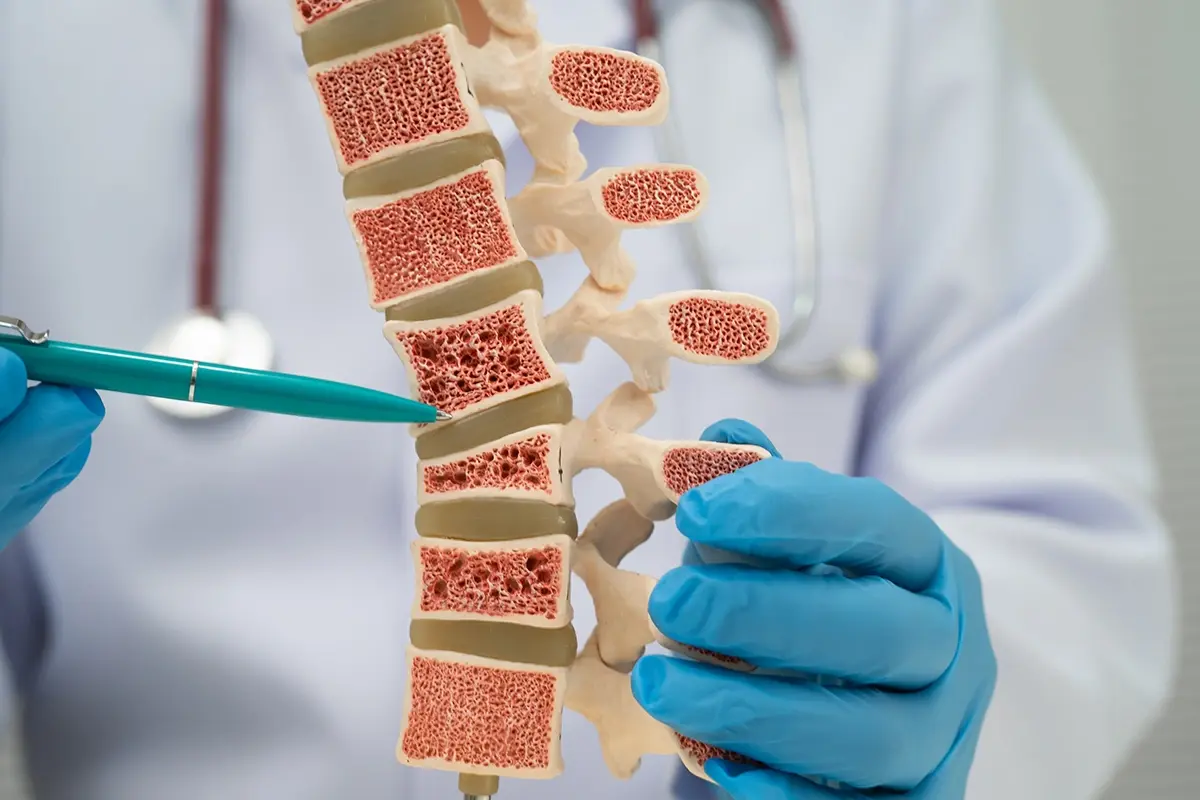
Osteoporosis
This condition reduces bone density and makes bones more fragile, increasing the risk of hip, spine and wrist fractures.
Advancing Age
Fractures become more common with age as bones gradually lose density and strength. This makes even minor falls more likely to result in injury.
Female Sex and Menopause
Women have a higher risk, especially after menopause. Lower oestrogen levels accelerate bone loss, increasing fracture risk over time.
Chronic Medical Conditions
Conditions such as chronic kidney disease, hormonal disorders and certain cancers can impair bone health and stability.
Medications
Long-term use of medications like corticosteroids may reduce bone strength or affect balance, increasing the risk of falls.
Lifestyle Factors
Smoking and a sedentary lifestyle contribute to reduced bone mass, muscle weakness and poorer balance, increasing fracture risk.
Geriatric Fractures We Treat
Common Types of Geriatric Fractures
The most common fractures in older adults include:
Hip Fractures (Neck of Femur Fractures, Inter-trochanteric Fractures)
Hip fractures are among the most serious injuries in the elderly and most often occur after a fall. They typically cause severe pain in the groin or thigh, and the individual may be unable to bear weight or walk. These fractures often require surgical treatment and hospitalisation.
Wrist Fractures (Distal Radius Fractures)
Wrist fractures commonly occur when a person falls onto an outstretched hand. Symptoms include pain, swelling, bruising and difficulty moving or gripping with the affected hand.
Vertebral Compression Fractures
These occur when weakened vertebrae collapse, sometimes after minimal trauma or even spontaneously. They may cause sudden back pain, reduced mobility and progressive loss of height.
Shoulder Fractures (Proximal Humerus Fractures)
Shoulder fractures typically result from a fall onto the arm or shoulder. They can cause significant pain, swelling and difficulty lifting or using the affected arm.
Understanding Your Evaluation
How Are Fractures in the Elderly Diagnosed?
Diagnosis usually begins with a review of your medical history and a careful physical examination. Your doctor will assess the area for tenderness, swelling, deformity and difficulty bearing weight. If needed, further tests may be recommended, including:
Understanding Your Evaluation
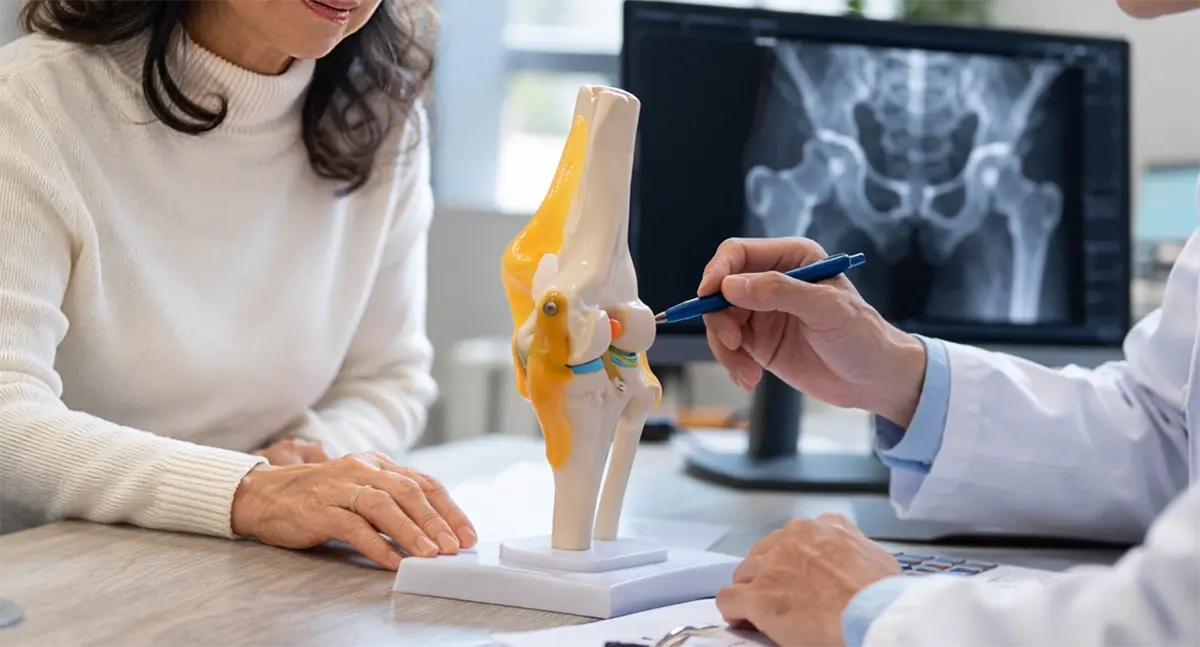
How Are Fractures in the Elderly Diagnosed?
Diagnosis usually begins with a review of your medical history and a careful physical examination. Your doctor will assess the area for tenderness, swelling, deformity and difficulty bearing weight. If needed, further tests may be recommended, including:
X-ray
An X-ray is typically the first imaging test performed. It helps confirm whether a bone is broken and shows the location and pattern of the fracture.
CT or MRI Scan
A CT scan provides detailed images of complex fractures, particularly around joints. An MRI scan is useful for detecting hairline fractures and assessing soft tissue or ligament injuries that may not be visible on X-ray.
Bone Mineral Density Scan (DEXA)
A DEXA scan measures bone mineral density. It is commonly performed after a fragility fracture to assess for osteoporosis and guide long-term treatment and fracture prevention strategies.
Geriatric Fracture Treatments in Singapore
The primary goals of geriatric fracture treatment are to relieve pain, stabilise the fracture, restore mobility and promote early rehabilitation. Prolonged bed rest is avoided whenever possible, as immobility increases the risk of complications such as pneumonia, urinary tract infections, deep vein thrombosis and pressure sores. Treatment depends on the type and severity of the fracture, as well as the patient’s overall health and functional goals. Management is broadly divided into non-surgical and surgical approaches.
Non-Surgical Treatment Options
Stable or minimally displaced fractures may be managed conservatively. This may include:
- Pain Relief Medication
Carefully selected analgesics are prescribed to control pain and enable mobilisation.
- Immobilisation
Braces, splints or casts help protect the fracture and maintain alignment during healing.
- Physiotherapy
Early, guided rehabilitation restores strength, balance and mobility while reducing complications from inactivity.
- Bone Health Optimisation
Calcium, vitamin D and osteoporosis medications may be initiated to reduce the risk of future fractures.
Surgical Treatment Options
Surgery may be required for displaced, unstable or function-limiting fractures. Procedures may include:
- Fracture Fixation
Plates, screws, rods or nails are used to stabilise the bone and allow earlier mobilisation.
- Hip Replacement
Partial hip replacement or total hip replacement may be performed for certain hip fractures to restore mobility and reduce pain.
- Spinal Procedures
Selected patients with persistent, severe pain from vertebral compression fractures may benefit from vertebroplasty or balloon kyphoplasty.
Regardless of treatment type, rehabilitation is essential. A structured recovery plan helps older patients regain safe movement, reduce complications, and return to daily activities more confidently.
Get Relief From Elderly (Geriatric) Fracture at HC Orthopaedic Surgery
Geriatric fractures require timely and coordinated care, particularly as bone fragility and medical complexity increase with age. Beyond stabilising the fracture itself, management should also address underlying osteoporosis, reduce fall risk and support early rehabilitation to preserve independence. With appropriate medical guidance and a structured recovery plan, many older adults can regain mobility and maintain their quality of life. Comprehensive osteoporosis screening and targeted bone health management play an important role in reducing the risk of first and subsequent fragility fractures, forming a key part of long-term prevention.

Get Relief From Elderly (Geriatric) Fracture at HC Orthopaedic Surgery
Geriatric fractures require timely and coordinated care, particularly as bone fragility and medical complexity increase with age. Beyond stabilising the fracture itself, management should also address underlying osteoporosis, reduce fall risk and support early rehabilitation to preserve independence. With appropriate medical guidance and a structured recovery plan, many older adults can regain mobility and maintain their quality of life. Comprehensive osteoporosis screening and targeted bone health management play an important role in reducing the risk of first and subsequent fragility fractures, forming a key part of long-term prevention.
Our Specialised Team
At HC Orthopaedic Surgery, comprehensive care for elderly fractures is led by Dr Henry Chan, Medical Director and senior consultant orthopaedic surgeon, together with Dr Nicholas Yeoh, Dr Toon Dong Hao and Dr Tang Zhi Hao. Our team provides thorough assessment, individualised fracture management and structured bone health optimisation tailored to each patient’s medical condition and functional goals.
Frequently Asked Questions (FAQs) About Geriatric Fractures
How soon can I go home after surgery for a geriatric fracture?
How soon will I be able to walk again?
What are the possible complications of geriatric fractures?
Can older adults recover well from fractures?
How long does it take to recover from a geriatric fracture?
How can fractures in the elderly be prevented?
What should I do if I fall?
Meet Our Specialist Team
Our team comprises Dr Henry Chan, Dr Nicholas Yeoh, Dr Toon Dong Hao, and Dr Tang Zhi Hao — experienced orthopaedic surgeons with subspecialty experience and a patient-centred approach to care.

Dr Henry Chan
Medical Director & Senior Consultant Orthopaedic Surgeon
MBBS (S’pore), MRCS (Edinburgh), MMed (Orthopaedic Surgery), FRCS (Edinburgh)
Dr Henry Chan is an experienced orthopaedic surgeon specialising in joint replacement and complex revision surgery. Trained at the renowned Helios Endo-Klinik in Germany under the MOH HMDP scholarship, he has performed over 1,000 joint replacements and specialises in computer-assisted and robotic joint replacement techniques for precise outcomes.

Dr Nicholas Yeoh
Senior Consultant Orthopaedic Surgeon
MBChB (Edinburgh), MRCS (Edinburgh), MMed (Orthopaedic Surgery), FRCS (Edinburgh)
Dr Nicholas Yeoh is an MOH-accredited orthopaedic specialist and Fellow of the Royal College of Surgeons of Edinburgh. Fellowship-trained in hip and knee reconstruction in Sydney under the MOH HMDP scholarship, he specialises in minimally invasive joint replacement, robotic surgery and advanced techniques that enhance recovery and surgical outcomes.

Dr Toon Dong Hao
Senior Consultant Orthopaedic Surgeon
MBChB (Leeds), MRCS (Edinburgh), MMed (Orthopaedic Surgery), FRCS (Edinburgh)
Dr Toon Dong Hao is a skilled orthopaedic surgeon and Fellow of the Royal College of Surgeons of Edinburgh. Fellowship-trained in Advanced Shoulder and Elbow Surgery in Sydney under the MOH HMDP scholarship, Dr Toon specialises in sports injuries, arthroscopic surgery and complex shoulder, elbow and knee procedures to restore function and mobility.

Dr Tang Zhi Hao
Senior Consultant Orthopaedic Surgeon
MBBS (S’pore), MRCS (Edinburgh), MMed (Orthopaedic Surgery), FRCS (Edinburgh)
Dr Tang Zhi Hao is a fellowship-trained orthopaedic surgeon specialising in foot and ankle conditions. He completed his Foot and Ankle Surgery fellowship at Severance Hospital, Yonsei University Health System in Seoul under Professor Jin Woo Lee. Prior to private practice, he served as Consultant and Deputy Head of Orthopaedics at Khoo Teck Puat Hospital.