Degenerative Disc Disease:
Symptoms, Causes and Treatments





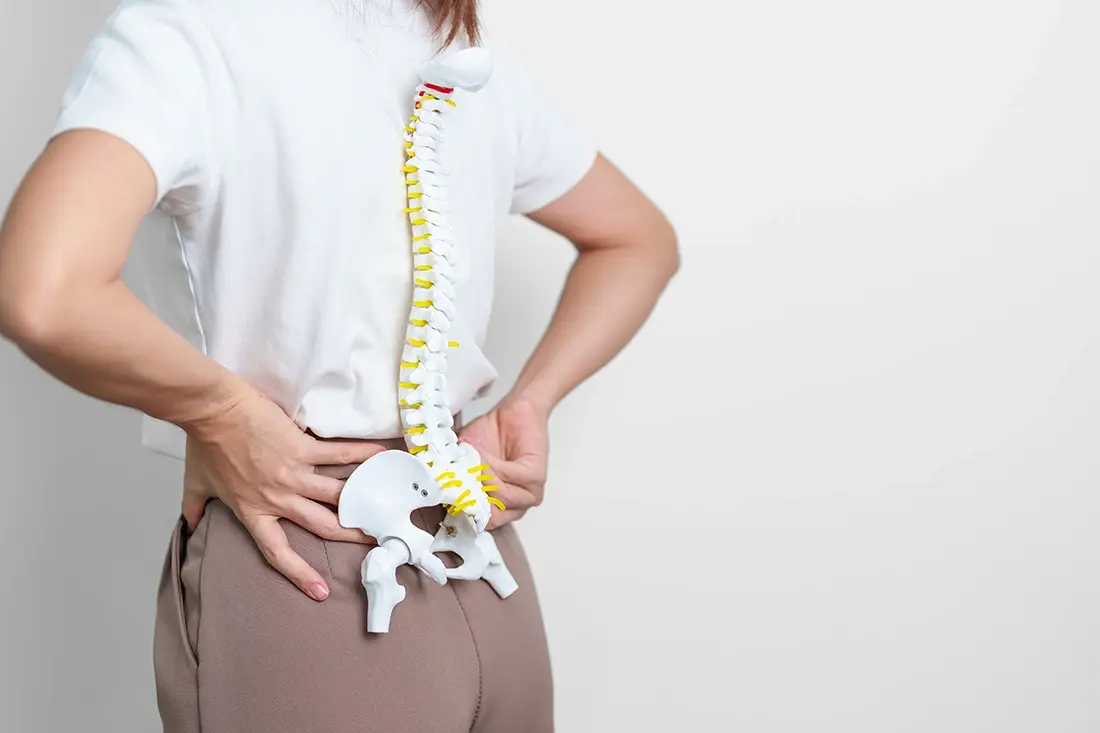
Degenerative disc disease (DDD) is a condition in which the intervertebral discs — the soft cushions between the bones of the spine — gradually lose hydration, elasticity, and height over time. As these discs wear down, they become less effective at absorbing shock and supporting spinal movement, which can lead to persistent neck or lower back pain.
Although disc degeneration is a natural part of ageing, it does not always cause symptoms. When it does, pain may develop due to inflammation, disc instability, or nerve compression. The severity and progression of symptoms vary depending on the level of the spine involved and the extent of disc changes.
At HC Orthopaedic Surgery, we provide comprehensive management for degenerative disc disease treatment. Our team is dedicated to improving your spinal health so you can return to your daily life with ease.
What Are the Common Symptoms of Degenerative Disc Disease?
Unlike an acute injury, the symptoms of degenerative disc disease often develop over several years. The pain is typically mechanical, meaning it fluctuates based on your activity and posture (e.g. sitting, bending, lifting, twisting).
Localised Back or Neck Pain
The primary symptom is a chronic, low-level ache in the neck or lower back. This discomfort often intensifies when you are in positions that put a high load on the discs, such as sitting for long periods or performing heavy lifting.
Muscle Spasms and Reduced Range of Motion
The body often tries to protect a degenerated disc by tightening the surrounding muscles. This results in painful spasms and a noticeable loss of flexibility, making it difficult to twist your torso or tilt your head comfortably.
Radiating Discomfort and Nerve Irritation
As a disc loses its height and structural integrity, it can lead to the narrowing of the spaces where nerves exit the spine. This can cause pain to "travel" into the buttocks or down the arms, often accompanied by a tingling sensation.
Increased Pain During Specific Movements
Many patients notice that their pain spikes during movements that involve twisting, bending, or lifting. Conversely, walking or lying down in a supported position often helps to temporarily alleviate the pressure on the affected discs.
Why It Happens
What Causes Degenerative Disc Disease?
Degenerative disc disease is not actually a "disease" in the traditional sense, but rather a condition where the spinal discs lose their ability to act as effective shock absorbers. Possible causes include:
Natural Loss of Fluid Content
Intervertebral discs are primarily composed of water. As we age, these discs naturally dry out and become thinner. This loss of fluid makes them less flexible and less capable of cushioning the vertebrae during movement.
Structural Micro-Tears
Daily activities and minor injuries can cause small tears in the tough outer layer of the disc. While the body attempts to repair these, the scar tissue that forms is often weaker and more prone to further damage, leading to a cycle of degradation.
Loss of Disc Height and Stability
As the disc flattens, the space between the vertebrae decreases. This changes the way the spinal joints (facet joints) interact, often leading to bone-on-bone friction and the development of painful bone spurs.
Know Your Risk Profile
What Are the Risk Factors for Degenerative Disc Disease?
Although age-related disc changes are common, several factors can increase mechanical stress on the spine and accelerate disc degeneration.
Long-Term Mechanical Stress
Engaging in high-impact sports or working in jobs that require repetitive heavy lifting can place excessive demands on the spinal discs. Over decades, this cumulative stress leads to earlier onset of degeneration.
Smoking and Nutritional Factors
Tobacco use reduces blood flow to the spinal structures, depriving the discs of nutrients they need to maintain their water content. This can speed up the drying-out process.
History of Spinal Injury
A single major injury, such as a fall or a vehicular accident, can compromise the structural integrity of a disc. Even if the initial injury heals, that disc may still degenerate faster than the others.
Where Degeneration Occurs
Types of Spinal Degeneration Patterns
Degenerative disc disease can affect different regions of the spine. The symptoms and functional impact often depend on whether the cervical (neck), thoracic (mid-back), or lumbar (lower back) discs are involved.
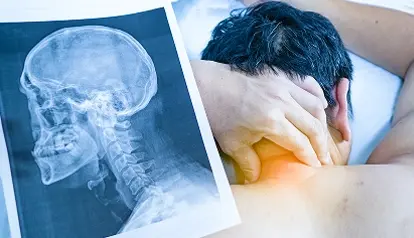
Cervical Degeneration (Neck)
When the discs in the neck wear down, it often leads to chronic stiffness and headaches. In some cases, it can cause radiating pain that affects the shoulders and hands.

Lumbar Degeneration (Lower Back)
The lower back carries the majority of your body weight, making it the most common site for disc wear. This often results in a deep ache in the small of the back that worsens after a long day of standing or sitting.
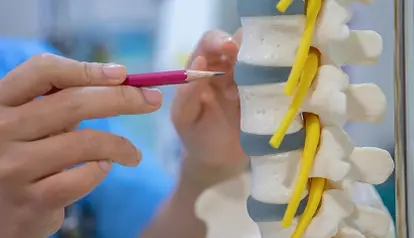
Multi-Level Degeneration
In many patients, the wear and tear is not limited to a single disc but affects several levels of the spine simultaneously. This requires a more holistic approach to rehabilitation and pain management.
Understanding Your Evaluation
How Is Degenerative Disc Disease Diagnosed?
Diagnosis focuses on determining whether disc degeneration is indeed responsible for your pain and identifying which level of the spine is affected. This involves assessing symptom patterns, spinal function, and structural changes within the discs.
Understanding Your Evaluation
How Is Degenerative Disc Disease Diagnosed?
Diagnosis focuses on determining whether disc degeneration is indeed responsible for your pain and identifying which level of the spine is affected. This involves assessing symptom patterns, spinal function, and structural changes within the discs.
Comprehensive Physical Assessment
A detailed physical examination is performed to assess spinal alignment, range of motion, and areas of tenderness. Muscle strength, reflexes, and sensation are also evaluated to determine whether disc degeneration is affecting nearby nerve roots.
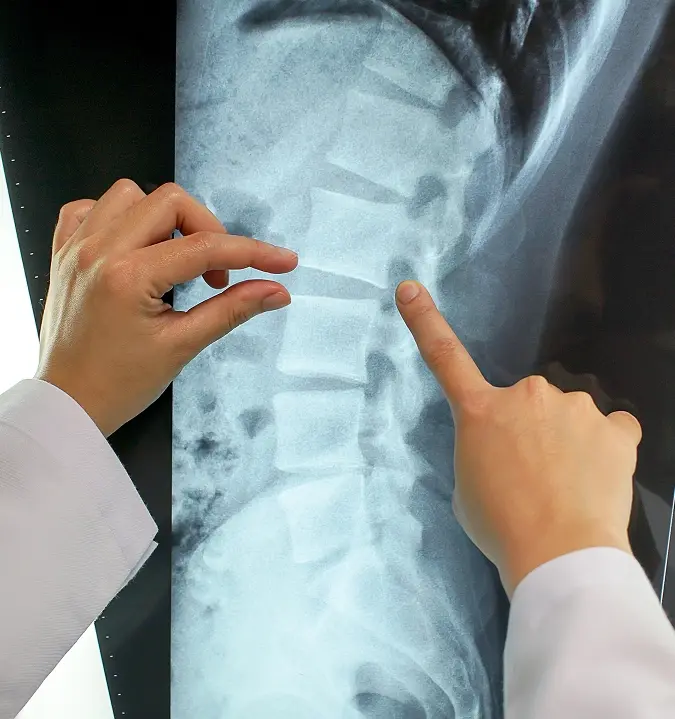
X-Ray and MRI Evaluation
X-rays are useful for identifying a loss of disc height and the presence of bone spurs. An MRI provides a much more detailed view, allowing us to see the exact water content of the discs and any related soft tissue issues.
Diagnostic Discography
In rare cases where the source of the pain is unclear, a specialised test may be performed to identify exactly which disc is responsible for your symptoms by temporarily increasing the pressure within the disc.
Exploring Treatment Options
Degenerative Disc Disease Treatments in Singapore
Treatment for degenerative disc disease is tailored to the severity of symptoms and the extent of disc degeneration. The primary goals are to relieve pain, maintain spinal stability, and preserve function. Most patients improve with conservative measures, while surgical intervention is considered only when symptoms persist or neurological complications develop.
Physiotherapy Exercises
The most effective long-term treatment is often a dedicated core-strengthening program. By building the muscles that support the spine, we can reduce the mechanical load placed on the degenerated discs.
Anti-Inflammatory and Pain Management
We utilise clinically-proven medications and localised injections to manage the inflammation that often accompanies disc wear. This helps to break the cycle of pain and muscle guarding.
Disc Replacement and Spinal Fusion
For advanced cases where conservative care is insufficient, surgical options may be considered. These range from replacing a worn-out disc with an artificial one to fusing two vertebrae together to eliminate painful movement in a specific joint.
Get Relief From Degenerative Disc Disease at HC Orthopaedic Surgery
Degenerative disc disease can make you feel as though your body is working against you, turning simple daily movements into a source of frustration. Because spinal wear is a progressive process, early intervention is the key to maintaining your long-term mobility and preventing more severe complications. A detailed clinical evaluation allows us to identify the specific levels of your spine that need support and to create a roadmap for your recovery.

Get Relief From Degenerative Disc Disease at HC Orthopaedic Surgery
Degenerative disc disease can make you feel as though your body is working against you, turning simple daily movements into a source of frustration. Because spinal wear is a progressive process, early intervention is the key to maintaining your long-term mobility and preventing more severe complications. A detailed clinical evaluation allows us to identify the specific levels of your spine that need support and to create a roadmap for your recovery.
Our Specialised Team
At HC Orthopaedic Surgery our specialists, including , Dr Henry Chan, Dr Nicholas Yeoh, Dr Toon Dong Hao and Dr Tang Zhi Hao, offer the expertise required to navigate complex spinal health challenges. We are committed to providing evidence-based, individualised care that focuses on your needs. Get in touch with us today to schedule your consultation and take a proactive step toward a more comfortable, active future.
Frequently Asked Questions (FAQs) About Degenerative Disc Disease
Is degenerative disc disease a permanent condition?
Can lifestyle changes really slow down disc degeneration?
Does everyone eventually get degenerative disc disease?
What kind of exercise is best for thinning discs?
When should surgery be considered for disc wear?
Meet Our Specialist Team
Our team comprises Dr Henry Chan, Dr Nicholas Yeoh, Dr Toon Dong Hao, and Dr Tang Zhi Hao — experienced orthopaedic surgeons with subspecialty experience and a patient-centred approach to care.

Dr Henry Chan
Medical Director & Senior Consultant Orthopaedic Surgeon
MBBS (S’pore), MRCS (Edinburgh), MMed (Orthopaedic Surgery), FRCS (Edinburgh)
Dr Henry Chan is an experienced orthopaedic surgeon specialising in joint replacement and complex revision surgery. Trained at the renowned Helios Endo-Klinik in Germany under the MOH HMDP scholarship, he has performed over 1,000 joint replacements and specialises in computer-assisted and robotic joint replacement techniques for precise outcomes.

Dr Nicholas Yeoh
Senior Consultant Orthopaedic Surgeon
MBChB (Edinburgh), MRCS (Edinburgh), MMed (Orthopaedic Surgery), FRCS (Edinburgh)
Dr Nicholas Yeoh is an MOH-accredited orthopaedic specialist and Fellow of the Royal College of Surgeons of Edinburgh. Fellowship-trained in hip and knee reconstruction in Sydney under the MOH HMDP scholarship, he specialises in minimally invasive joint replacement, robotic surgery and advanced techniques that enhance recovery and surgical outcomes.

Dr Toon Dong Hao
Senior Consultant Orthopaedic Surgeon
MBChB (Leeds), MRCS (Edinburgh), MMed (Orthopaedic Surgery), FRCS (Edinburgh)
Dr Toon Dong Hao is a skilled orthopaedic surgeon and Fellow of the Royal College of Surgeons of Edinburgh. Fellowship-trained in Advanced Shoulder and Elbow Surgery in Sydney under the MOH HMDP scholarship, Dr Toon specialises in sports injuries, arthroscopic surgery and complex shoulder, elbow and knee procedures to restore function and mobility.

Dr Tang Zhi Hao
Senior Consultant Orthopaedic Surgeon
MBBS (S’pore), MRCS (Edinburgh), MMed (Orthopaedic Surgery), FRCS (Edinburgh)
Dr Tang Zhi Hao is a fellowship-trained orthopaedic surgeon specialising in foot and ankle conditions. He completed his Foot and Ankle Surgery fellowship at Severance Hospital, Yonsei University Health System in Seoul under Professor Jin Woo Lee. Prior to private practice, he served as Consultant and Deputy Head of Orthopaedics at Khoo Teck Puat Hospital.