Shoulder Osteoarthritis:
Symptoms, Causes and Treatments






A dull ache in the shoulder that lingers after activity. Stiffness when reaching overhead or fastening a seatbelt. A gradual loss of movement that makes simple tasks feel harder than they used to. These changes are often dismissed as part of ageing, but they may signal shoulder osteoarthritis.
Shoulder osteoarthritis develops when the smooth cartilage that cushions the joint gradually wears down, causing friction, inflammation and progressive stiffness. Over time, this can affect sleep, work and everyday function. Recognising the early signs and understanding the available treatment options can help you take steps to relieve pain, preserve movement and maintain an active lifestyle.
What Is Shoulder Osteoarthritis?
Shoulder osteoarthritis is a condition in which the cartilage that cushions the shoulder joint gradually breaks down. Cartilage normally allows the ball and socket of the shoulder to glide smoothly during movement. When this protective layer wears away, the bones begin to rub against each other, leading to pain, stiffness and inflammation.
As the condition progresses, the joint space may narrow and bony growths known as bone spurs can develop. These changes can restrict movement and make everyday activities such as reaching, lifting or dressing increasingly difficult. Shoulder osteoarthritis typically develops over time and may worsen without appropriate management.
What Are the Symptoms of Shoulder Osteoarthritis?
Shoulder osteoarthritis often develops gradually, with symptoms that may worsen over time. The severity can vary depending on the extent of cartilage wear and joint inflammation.
Shoulder Pain
Pain is the most common symptom. It may begin as a dull ache during or after activity and gradually become more persistent. As the condition progresses, pain may occur even at rest or at night, sometimes affecting sleep.
Stiffness
The shoulder may feel tight, especially after periods of inactivity. Morning stiffness or difficulty moving the arm after sitting for some time is common.
Reduced Range of Motion
As cartilage wears down and the joint space narrows, movements such as reaching overhead, rotating the arm or fastening clothing behind the back may become limited.
Grinding or Clicking Sensation
Some individuals notice a grinding, grating or clicking sound when moving the shoulder. This occurs when rough joint surfaces move against each other.
Weakness
Pain and reduced joint function may lead to a feeling of weakness in the shoulder, particularly during lifting or overhead activities.
What Causes and Contributes to Shoulder Osteoarthritis?
Shoulder osteoarthritis most commonly develops as a result of gradual cartilage wear over time rather than a single identifiable event. In many individuals, it reflects a combination of age-related degeneration and cumulative mechanical stress on the joint. However, certain conditions can accelerate or directly contribute to cartilage breakdown.
Age-related Degeneration
As we age, the cartilage that cushions the shoulder joint gradually loses elasticity and resilience. Over time, repeated movement and daily use can lead to thinning of the joint surface and progressive degeneration.
Previous Shoulder Injury
Fractures involving the joint surface, severe dislocations or cartilage injuries can disrupt normal joint mechanics. Even after healing, these changes may increase the risk of developing post-traumatic osteoarthritis.
Chronic Rotator Cuff Tears
Long-standing rotator cuff tears can alter the balance and alignment of the shoulder joint. This abnormal movement pattern may accelerate cartilage wear, a condition sometimes referred to as rotator cuff arthropathy.
Repetitive Overuse
Frequent overhead activity, heavy lifting or high-demand sports can place sustained stress on the shoulder joint, contributing to gradual cartilage breakdown over time.
Inflammatory or Systemic Conditions
Inflammatory arthritis and certain metabolic conditions can damage joint structures or promote chronic inflammation, increasing the likelihood of secondary osteoarthritis.
Understanding the Differences
Types of Shoulder Osteoarthritis
Shoulder osteoarthritis can be broadly classified based on its underlying cause and the pattern of joint damage. Identifying the type helps guide treatment decisions and long-term management.

Primary Osteoarthritis
Primary osteoarthritis develops gradually without a specific triggering injury. It is typically age-related and results from progressive cartilage wear over time. This form most commonly affects the main shoulder joint, known as the glenohumeral joint.
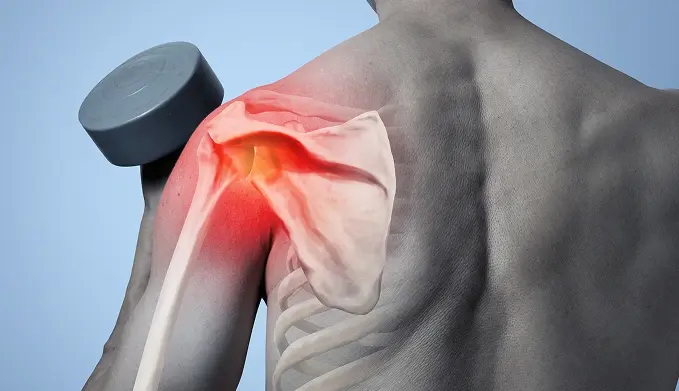
Post-traumatic Osteoarthritis
This type occurs following a significant shoulder injury, such as a fracture involving the joint surface or a severe dislocation. Even after the initial injury has healed, altered joint mechanics may lead to accelerated cartilage degeneration.
Rotator Cuff Tear Arthropathy
In cases of long-standing or massive rotator cuff tears, the normal balance of the shoulder joint is disrupted. This can cause abnormal contact between the bones, leading to progressive joint degeneration and arthritis associated with weakness and instability.
At HC Orthopaedic Surgery, our team of shoulder specialists has the clinical expertise to treat all types of shoulder osteoarthritis with tailored, stage-appropriate care.
Understanding Your Evaluation
How Is Shoulder Osteoarthritis Diagnosed?
Diagnosis of shoulder osteoarthritis begins with a detailed clinical evaluation. Your doctor will review your symptoms, assess how they have progressed over time and examine the shoulder for pain, stiffness and range of motion limitations.
Understanding Your Evaluation
How Is Shoulder Osteoarthritis Diagnosed?
Diagnosis of shoulder osteoarthritis begins with a detailed clinical evaluation. Your doctor will review your symptoms, assess how they have progressed over time and examine the shoulder for pain, stiffness and range of motion limitations.
Physical Examination
During the examination, the shoulder is assessed for tenderness, crepitus, joint swelling and restriction of movement. Strength testing may also be performed to evaluate for associated rotator cuff involvement.
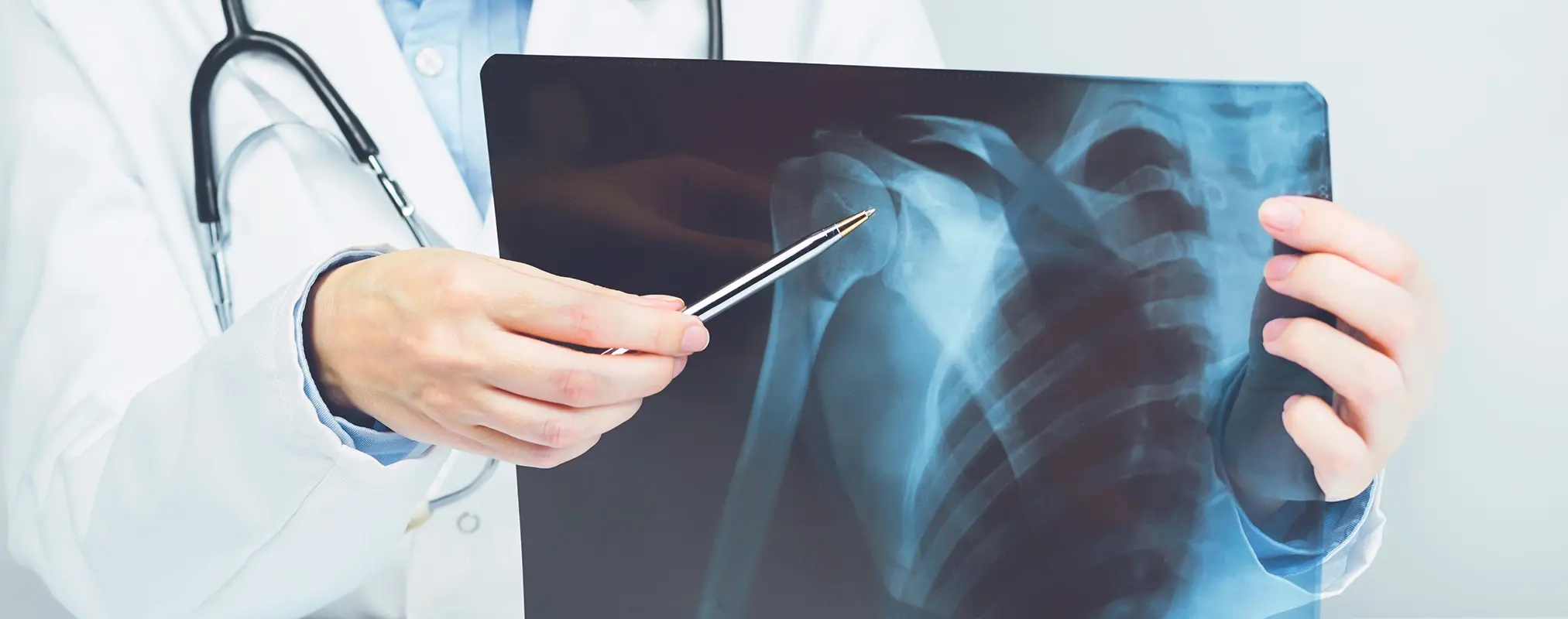
X-rays
X-rays are the primary imaging tool used to confirm shoulder osteoarthritis. They can show narrowing of the joint space, bone spurs and changes in bone structure that indicate cartilage loss.
Advanced Imaging
In selected cases, MRI or CT scans may be recommended to evaluate soft tissue structures, assess rotator cuff integrity or better understand complex joint changes before planning treatment.
Joint Fluid Analysis: In some cases, fluid from the joint may be extracted and analysed. This can provide additional information about the type of arthritis and the severity of the condition.
Shoulder Osteoarthritis Treatments in Singapore
Treatment for shoulder osteoarthritis aims to relieve pain, maintain or improve range of motion and support ongoing shoulder function. Management is tailored to the severity of symptoms, imaging findings and individual activity goals, with non-surgical options often tried before more invasive interventions.
Non-Surgical Treatments
Activity Modification
Avoiding repetitive overhead movements, heavy lifting or activities that aggravate pain can reduce stress on the joint and improve comfort.
Physiotherapy
A structured rehabilitation programme helps preserve range of motion, strengthen the rotator cuff and surrounding muscles, and improve overall shoulder mechanics.
Medications and Pain Relief
Oral analgesics or anti-inflammatory medications may be prescribed to help manage pain and inflammation, particularly during flare-ups.
Injection Therapy
Corticosteroid injections can reduce inflammation and relieve pain. In selected cases, hyaluronic acid injections may help improve joint lubrication and movement.
Surgical Treatments
Arthroscopic Debridement
For selected patients with mechanical symptoms, minimally invasive arthroscopic surgery can be used to remove loose fragments and smooth rough joint surfaces.
Joint Replacement Surgery (Arthroplasty)
In advanced cases where conservative treatments have not provided adequate relief, shoulder replacement surgery allows the damaged joint surfaces to be replaced with artificial components, significantly reducing pain and improving function.
Your Recovery Journey
What Is the Recovery Timeline for Shoulder Osteoarthritis?
Shoulder osteoarthritis is a chronic condition, so recovery focuses on symptom control and functional improvement rather than complete reversal of joint changes. The timeline varies depending on severity and the type of treatment received.
For patients managed non-surgically, symptom improvement may occur gradually over several weeks with physiotherapy, activity modification and medication. Flare-ups can happen intermittently, but consistent rehabilitation helps maintain mobility and reduce pain.
If surgery is performed, recovery follows a structured rehabilitation plan. After arthroscopic procedures, improvement may be seen within a few months. Following shoulder replacement surgery, rehabilitation typically progresses over several months, with gradual return to daily activities and continued gains in strength and function over time.
Manage Shoulder Osteoarthritis at HC Orthopaedic Surgery
Shoulder osteoarthritis can gradually erode comfort, mobility and independence if left unaddressed. While the condition progresses over time, early recognition and a structured, stage-appropriate approach can significantly reduce pain, preserve joint function and delay more advanced degeneration. With the right combination of conservative care and, when necessary, surgical intervention, many individuals are able to maintain an active and functional lifestyle.

Manage Shoulder Osteoarthritis at HC Orthopaedic Surgery
Shoulder osteoarthritis can gradually erode comfort, mobility and independence if left unaddressed. While the condition progresses over time, early recognition and a structured, stage-appropriate approach can significantly reduce pain, preserve joint function and delay more advanced degeneration. With the right combination of conservative care and, when necessary, surgical intervention, many individuals are able to maintain an active and functional lifestyle.
Our Specialised Team
At HC Orthopaedic Surgery, care is led by Medical Director and Senior Consultant Orthopaedic Surgeon Dr Henry Chan, together with Dr Nicholas Yeoh, Dr Toon Dong Hao and Dr Tang Zhi Hao. In particular, Dr Toon completed a fellowship in Advanced Shoulder and Elbow Surgery in Sydney, Australia, and brings dedicated subspecialty expertise in complex shoulder reconstruction and joint replacement procedures for advanced osteoarthritis. Explore safe ways to regain mobility and reduce discomfort with us today.
Frequently Asked Questions (FAQs) About Shoulder Osteoarthritis
Can shoulder osteoarthritis get worse over time?
Will physiotherapy help my shoulder osteoarthritis?
When should I consider surgery for shoulder osteoarthritis?
Can lifestyle changes help manage shoulder osteoarthritis?
Is shoulder osteoarthritis common in younger adults?
Are injections an option for shoulder osteoarthritis treatment?
Does shoulder osteoarthritis always affect both shoulders?
How is shoulder osteoarthritis different from other shoulder conditions?
Meet Our Specialist Team
Our team comprises Dr Henry Chan, Dr Nicholas Yeoh, Dr Toon Dong Hao, and Dr Tang Zhi Hao — experienced orthopaedic surgeons with subspecialty experience and a patient-centred approach to care.

Dr Henry Chan
Medical Director & Senior Consultant Orthopaedic Surgeon
MBBS (S’pore), MRCS (Edinburgh), MMed (Orthopaedic Surgery), FRCS (Edinburgh)
Dr Henry Chan is an experienced orthopaedic surgeon specialising in joint replacement and complex revision surgery. Trained at the renowned Helios Endo-Klinik in Germany under the MOH HMDP scholarship, he has performed over 1,000 joint replacements and specialises in computer-assisted and robotic joint replacement techniques for precise outcomes.

Dr Nicholas Yeoh
Senior Consultant Orthopaedic Surgeon
MBChB (Edinburgh), MRCS (Edinburgh), MMed (Orthopaedic Surgery), FRCS (Edinburgh)
Dr Nicholas Yeoh is an MOH-accredited orthopaedic specialist and Fellow of the Royal College of Surgeons of Edinburgh. Fellowship-trained in hip and knee reconstruction in Sydney under the MOH HMDP scholarship, he specialises in minimally invasive joint replacement, robotic surgery and advanced techniques that enhance recovery and surgical outcomes.

Dr Toon Dong Hao
Senior Consultant Orthopaedic Surgeon
MBChB (Leeds), MRCS (Edinburgh), MMed (Orthopaedic Surgery), FRCS (Edinburgh)
Dr Toon Dong Hao is a skilled orthopaedic surgeon and Fellow of the Royal College of Surgeons of Edinburgh. Fellowship-trained in Advanced Shoulder and Elbow Surgery in Sydney under the MOH HMDP scholarship, Dr Toon specialises in sports injuries, arthroscopic surgery and complex shoulder, elbow and knee procedures to restore function and mobility.

Dr Tang Zhi Hao
Senior Consultant Orthopaedic Surgeon
MBBS (S’pore), MRCS (Edinburgh), MMed (Orthopaedic Surgery), FRCS (Edinburgh)
Dr Tang Zhi Hao is a fellowship-trained orthopaedic surgeon specialising in foot and ankle conditions. He completed his Foot and Ankle Surgery fellowship at Severance Hospital, Yonsei University Health System in Seoul under Professor Jin Woo Lee. Prior to private practice, he served as Consultant and Deputy Head of Orthopaedics at Khoo Teck Puat Hospital.