Dislocated Shoulder:
Types, Treatment and Recovery






A sudden fall, an awkward tackle or even bracing yourself during a slip can result in an intense, unmistakable pain in the shoulder. The arm may look out of place, feel unstable or become impossible to move. A dislocated shoulder is not just painful, it can disrupt work, sport and everyday activities in an instant. Because the shoulder is designed for flexibility rather than deep stability, it is particularly vulnerable to being forced out of position.
Beyond the immediate pain, a shoulder dislocation may affect the surrounding ligaments, cartilage and muscles, increasing the risk of future instability if not properly managed. Understanding the different types of dislocation, available treatment options and what recovery entails is essential to restoring strength, confidence and long-term joint stability.
Anatomy of the Shoulder
The shoulder is a complex joint designed to prioritise movement over stability. It is formed by the ball-shaped head of the upper arm bone, known as the humerus, and the shallow socket of the shoulder blade, called the glenoid. This ball-and-socket arrangement allows the arm to move in multiple directions, including lifting, rotating and reaching overhead.
Stability is supported by a combination of soft tissues. The labrum, a ring of cartilage around the socket, helps deepen the joint and improve alignment. Surrounding ligaments and the joint capsule provide structural support, while the rotator cuff muscles and tendons actively stabilise the shoulder during movement. When significant force overwhelms these stabilising structures, the ball can slip partially or completely out of the socket, resulting in a shoulder dislocation.
What Are the Signs and Symptoms of a Dislocated Shoulder?
A dislocated shoulder often causes sudden and intense pain following a fall, collision or forceful movement. The discomfort is usually immediate and may be severe enough to limit any attempt to move the arm. Common signs and symptoms include:
- Visible deformity
The shoulder may appear squared off or out of place, with a noticeable change in contour.
- Severe pain
Pain typically worsens with movement and may radiate down the arm.
- Inability to move the arm
The arm may feel locked or extremely unstable.
- Swelling or bruising
Soft tissue injury around the joint can lead to visible swelling.
- Numbness or tingling
In some cases, nearby nerves may be affected, causing altered sensation in the shoulder, arm or hand.
Understanding the Differences
Different Types of Shoulder Dislocation
Shoulder dislocations are classified according to the direction in which the head of the humerus moves out of the shoulder socket. The direction of displacement influences both symptoms and treatment.Shoulder dislocations are classified according to the direction in which the head of the humerus moves out of the shoulder socket. The direction of displacement influences both symptoms and treatment.
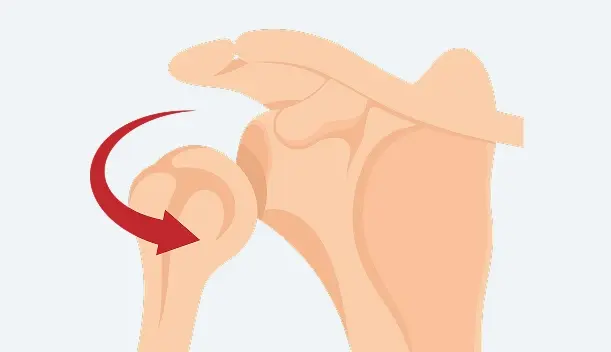
Anterior Dislocation
This is the most common type, accounting for the majority of shoulder dislocations. The humeral head is displaced forward, often when the arm is extended and rotated outward, such as during a fall onto an outstretched arm.
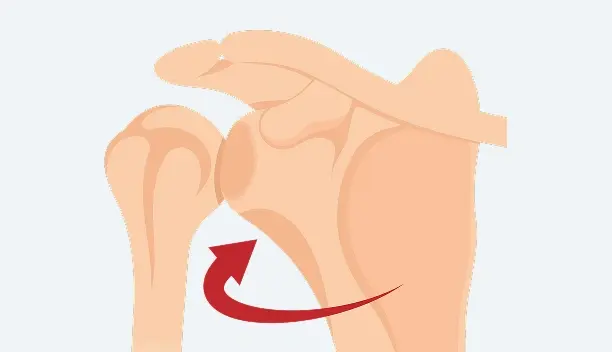
Posterior Dislocation
Less common than anterior dislocations, this type occurs when the humeral head is displaced backward. It is often associated with seizures, electrical injuries or high-impact trauma and may be less visibly obvious.
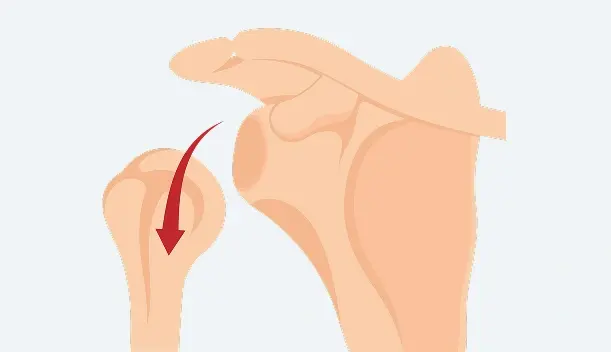
Inferior Dislocation
This rare form involves downward displacement of the humeral head, usually following severe trauma. The arm may be fixed in an elevated position, and urgent medical treatment is required.
Causes and Risk Factors of Shoulder Dislocation
A shoulder dislocation typically occurs when significant force pushes the head of the humerus out of the shoulder socket. However, certain factors can increase the likelihood of this injury or make recurrence more likely.
Traumatic Causes
Sports Injuries
Contact sports or forceful overhead movements can drive the shoulder out of position, particularly when the arm is extended or rotated outward.
Falls
Falling onto an outstretched arm or directly onto the shoulder is a common cause, especially during slips or loss of balance.
High-impact Accidents
Motor vehicle collisions or other severe trauma can generate enough force to dislocate the joint and may also injure surrounding ligaments or cartilage.
Seizures or Electrical Injuries
Sudden, intense muscle contractions during seizures or electrical shocks can cause posterior shoulder dislocations.
Risk Factors
Previous Shoulder Dislocation
Once the shoulder has dislocated, the stabilising structures may be stretched or torn, increasing the risk of recurrence.
Younger Age
Younger individuals, particularly those under 25, have a higher risk of recurrent instability after a first dislocation.
Participation in Contact or Overhead Sports
Regular involvement in activities that place repeated stress on the shoulder increases susceptibility.
Ligament Laxity or Joint Hypermobility
People with naturally looser ligaments may be more prone to shoulder instability.
Risks of Delayed Care
Possible Complications of a Dislocated Shoulder
If a dislocated shoulder is not properly treated or rehabilitated, several complications may occur, particularly in active individuals or those with recurrent instability.
Recurrent Dislocations
Once the shoulder has dislocated, the stabilising ligaments and labrum may remain stretched or torn, increasing the risk of future episodes. Recurrence is more common in younger patients and those participating in contact or overhead sports.
Nerve or Blood Vessel Injury
In some cases, surrounding nerves or blood vessels may be affected during the injury. Symptoms can include numbness, tingling, weakness or changes in circulation in the arm or hand. Although uncommon, these injuries require prompt medical evaluation.
Persistent Stiffness
Inadequate rehabilitation or prolonged immobilisation may lead to reduced range of motion and shoulder stiffness. Structured physiotherapy is essential to restore mobility while maintaining stability.
Post-traumatic Arthritis
Repeated dislocations or significant cartilage damage can increase the risk of developing shoulder arthritis over time. This may result in chronic pain and reduced joint function later in life.
At HC Orthopaedic Surgery, our shoulder specialists provide stability-focused care for shoulder dislocations, delivering precise diagnosis and tailored treatment to restore strength and prevent recurrence.
Understanding Your Evaluation
How Is a Dislocated Shoulder Diagnosed?
Understanding Your Evaluation
How Is a Dislocated Shoulder Diagnosed?
A dislocated shoulder is usually diagnosed through a combination of clinical evaluation and imaging studies. The doctor will assess how the injury occurred, the severity of pain and whether there is visible deformity or restricted movement.
Physical Examination
During physical examination, the shoulder is carefully inspected for abnormal contour, swelling and tenderness. Range of motion is assessed cautiously, and nerve function may be checked to ensure there is no associated injury affecting sensation or circulation in the arm.
X-rays
X-rays are routinely performed to confirm the direction of dislocation and to identify any associated fractures. In certain cases, additional imaging such as MRI may be recommended to evaluate soft tissue injuries, including damage to the labrum, ligaments or rotator cuff.
Dislocated Shoulder Treatments in Singapore
Treatment depends on how severe the dislocation is. Most shoulder dislocations can be treated without surgery.
Immediate Management
After a dislocation, prompt medical attention is essential. The first step is a closed reduction, a controlled manoeuvre performed by a clinician to guide the humeral head back into its proper position. Pain relief and muscle relaxation are used to make the procedure as comfortable as possible. Once the joint is relocated, the arm is typically immobilised in a sling for a period to allow initial healing.
Surgical Treatment
Surgery may be considered in cases of recurrent dislocation, significant labral tears, bone loss or persistent instability despite rehabilitation. Arthroscopic stabilisation procedures are commonly performed to repair damaged structures and restore joint stability.
Non-Surgical Treatments
After reduction, treatment focuses on reducing pain and inflammation and restoring strength and movement:
Immobilisation
The shoulder is supported in a sling for a brief period, typically one to three weeks, depending on age and injury severity. Prolonged immobilisation is avoided to reduce the risk of stiffness.
Physiotherapy
Once the pain improves, exercises help the shoulder regain movement and strength, with added physiotherapy lowering the chance of the shoulder dislocating again.
Pain Management
Oral analgesics or anti-inflammatory medication may be prescribed. Ice therapy during the early phase can help reduce swelling and discomfort.
What Is the Recovery Time for a Dislocated Shoulder?
Recovery time after a dislocated shoulder varies depending on the severity of the injury, whether it is a first-time or recurrent dislocation, and the treatment approach used.
For uncomplicated first-time dislocations managed non-surgically, initial healing typically takes a few weeks. A sling is usually worn for a short period, followed by structured physiotherapy to restore range of motion and strengthen the shoulder. Most patients can gradually return to light daily activities within several weeks, while full return to sports or physically demanding work may take two to three months.
If surgery is required to repair torn ligaments or stabilise the joint, recovery is longer and follows a staged rehabilitation programme. Immobilisation is followed by progressive physiotherapy, and return to contact sports may take several months. Adhering to rehabilitation guidance is essential to regain stability and reduce the risk of recurrence.
How to Prevent Shoulder Dislocation
While not all shoulder dislocations can be prevented, especially those caused by sudden trauma, certain measures may reduce the risk of injury or recurrence.
Strengthening Exercises
Building strength in the rotator cuff and surrounding shoulder muscles helps improve joint stability. Targeted strengthening and conditioning programmes are particularly important for athletes and individuals involved in overhead or contact sports.
Proper Technique and Training
Using correct form during sports, weight training or repetitive overhead activities can reduce unnecessary strain on the shoulder joint. Gradual progression in intensity also lowers injury risk.
Protective Equipment
In contact sports, appropriate protective gear may help reduce the impact of falls or collisions.
Rehabilitation After Injury
After a first dislocation, completing a structured physiotherapy programme is essential. Adequate rehabilitation strengthens stabilising muscles and may reduce the likelihood of recurrent instability.
Activity Modification
Avoiding high-risk movements or positions, especially during early recovery, helps protect the healing structures of the shoulder.
Dislocated Shoulder Treatment at HC Orthopaedic Surgery
A dislocated shoulder is more than a momentary injury. Without accurate assessment and structured management, it can lead to ongoing instability, recurrent episodes and long-term joint damage. From recognising early symptoms to understanding treatment pathways and rehabilitation, timely care plays a critical role in restoring confidence, strength and safe return to daily activities or sport.

Dislocated Shoulder Treatment at HC Orthopaedic Surgery
A dislocated shoulder is more than a momentary injury. Without accurate assessment and structured management, it can lead to ongoing instability, recurrent episodes and long-term joint damage. From recognising early symptoms to understanding treatment pathways and rehabilitation, timely care plays a critical role in restoring confidence, strength and safe return to daily activities or sport.
Our Specialised Team
HC Orthopaedic Surgery is led by Medical Director and Senior Consultant Orthopaedic Surgeon Dr Henry Chan. Together with Dr Nicholas Yeoh, Dr Toon Dong Hao and Dr Tang Zhi Hao, the team provides comprehensive care for both first-time and recurrent dislocations. In particular, Dr Toon completed a fellowship in Advanced Shoulder and Elbow Surgery in Sydney, Australia, and brings dedicated subspecialty expertise in shoulder stabilisation and arthroscopic management of complex instability, further strengthening the team’s capabilities in advanced shoulder care.
Frequently Asked Questions (FAQs) About Shoulder Dislocation
How do I know if my shoulder is dislocated?
Is a dislocated shoulder an emergency?
Do I need surgery for a dislocated shoulder?
How long does it take to recover from a dislocated shoulder?
Can a dislocated shoulder happen again?
How do I prevent a dislocated shoulder from happening again?
Meet Our Specialist Team
Our team comprises Dr Henry Chan, Dr Nicholas Yeoh, Dr Toon Dong Hao, and Dr Tang Zhi Hao — experienced orthopaedic surgeons with subspecialty experience and a patient-centred approach to care.

Dr Henry Chan
Medical Director & Senior Consultant Orthopaedic Surgeon
MBBS (S’pore), MRCS (Edinburgh), MMed (Orthopaedic Surgery), FRCS (Edinburgh)
Dr Henry Chan is an experienced orthopaedic surgeon specialising in joint replacement and complex revision surgery. Trained at the renowned Helios Endo-Klinik in Germany under the MOH HMDP scholarship, he has performed over 1,000 joint replacements and specialises in computer-assisted and robotic joint replacement techniques for precise outcomes.

Dr Nicholas Yeoh
Senior Consultant Orthopaedic Surgeon
MBChB (Edinburgh), MRCS (Edinburgh), MMed (Orthopaedic Surgery), FRCS (Edinburgh)
Dr Nicholas Yeoh is an MOH-accredited orthopaedic specialist and Fellow of the Royal College of Surgeons of Edinburgh. Fellowship-trained in hip and knee reconstruction in Sydney under the MOH HMDP scholarship, he specialises in minimally invasive joint replacement, robotic surgery and advanced techniques that enhance recovery and surgical outcomes.

Dr Toon Dong Hao
Senior Consultant Orthopaedic Surgeon
MBChB (Leeds), MRCS (Edinburgh), MMed (Orthopaedic Surgery), FRCS (Edinburgh)
Dr Toon Dong Hao is a skilled orthopaedic surgeon and Fellow of the Royal College of Surgeons of Edinburgh. Fellowship-trained in Advanced Shoulder and Elbow Surgery in Sydney under the MOH HMDP scholarship, Dr Toon specialises in sports injuries, arthroscopic surgery and complex shoulder, elbow and knee procedures to restore function and mobility.

Dr Tang Zhi Hao
Senior Consultant Orthopaedic Surgeon
MBBS (S’pore), MRCS (Edinburgh), MMed (Orthopaedic Surgery), FRCS (Edinburgh)
Dr Tang Zhi Hao is a fellowship-trained orthopaedic surgeon specialising in foot and ankle conditions. He completed his Foot and Ankle Surgery fellowship at Severance Hospital, Yonsei University Health System in Seoul under Professor Jin Woo Lee. Prior to private practice, he served as Consultant and Deputy Head of Orthopaedics at Khoo Teck Puat Hospital.