Hip Osteoarthritis:
Symptoms, Causes & Treatment






Hip osteoarthritis (OA) is a chronic degenerative joint condition in which the protective cartilage lining the hip joint gradually wears down over time. As this cushioning layer deteriorates, the joint surfaces begin to rub against each other, leading to pain, stiffness, and reduced mobility.
The condition often develops slowly and may worsen over time, making everyday activities such as walking, climbing stairs, or standing for prolonged periods increasingly difficult. Hip osteoarthritis is a common cause of joint pain in older adults, although it can also affect younger individuals with previous injuries, structural abnormalities, or other risk factors.
Understanding Hip Joint
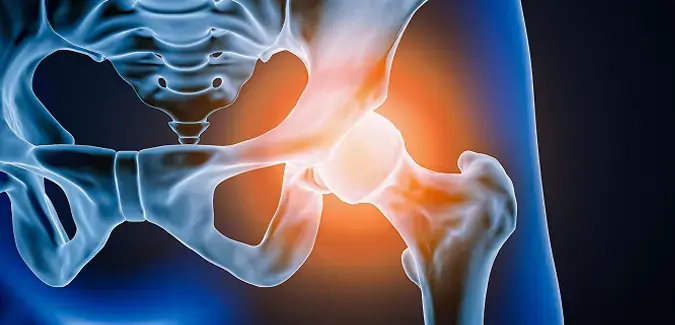
The Anatomy of the Hip Joint
The hip is a ball-and-socket joint where the femoral head (ball) fits into the acetabulum (socket) of the pelvis. This structure allows the hip to move in multiple directions while supporting the body’s weight during activities such as walking, standing, and climbing stairs. The joint surfaces are covered with articular cartilage, which provides a smooth, low-friction surface for movement and helps absorb impact. In osteoarthritis, this cartilage gradually wears down, leading to increased friction between the bones, inflammation, and progressive joint degeneration.
What Are the Common Symptoms of Hip Osteoarthritis?
As hip osteoarthritis progresses, the joint becomes less able to move smoothly and comfortably. This can lead to pain, stiffness, and reduced flexibility that make everyday activities such as walking, bending, or climbing stairs increasingly difficult.
Pain
Typically localised to the groin, thigh, or buttock; worsens with activity and improves with rest.
Stiffness
Particularly noticeable after periods of inactivity or in the morning.
Limited Range of Motion
Difficulty in movements like bending, squatting, or rotating the leg.
Crepitus
Grinding or clicking sensation during movement.
Functional Impairment
Difficulty in walking, climbing stairs, or performing daily tasks.
Why It Happens
What Causes Hip Osteoarthritis?
Hip osteoarthritis is primarily caused by the gradual breakdown of cartilage in the hip joint, which leads to friction between bones. Other possible causes include:
Trauma or Injury
Fractures, dislocations, or prior hip injuries can lead to post-traumatic osteoarthritis by directly damaging cartilage.
Congenital or Developmental Conditions
Structural abnormalities such as hip dysplasia cause uneven joint loading, leading to early cartilage breakdown.
Inflammatory Arthritis
Conditions like rheumatoid arthritis cause chronic inflammation that damages cartilage and accelerates joint degeneration.
Know Your Risk Profile
What Are the Risk Factors For Hip Osteoarthritis?
Hip osteoarthritis develops when long-term stress on the hip joint gradually damages the cartilage that cushions it. While ageing is a major contributor, several biological and lifestyle factors can increase the likelihood of cartilage breakdown and accelerate joint degeneration.
Ageing
Wear and tear over time makes older adults more susceptible.
Joint Overuse
Repetitive stress from physical labour or high-impact sports increases joint strain.
Obesity
Increased weight places excessive stress on the hip joint.
Genetics
A family history of osteoarthritis raises the risk of developing the condition.
What are the Grades of Hip Osteoarthritis?
Grade 1 (Mild)
Grade 2 (Early to Moderate)
Grade 3 (Moderate to Severe)
Joint space narrowing becomes more obvious, indicating greater cartilage loss. Bone changes are more pronounced, and inflammation may be present. Pain, stiffness, and reduced mobility are more frequent.
Grade 4 (Severe)
There is severe cartilage loss and significant joint damage. The bones may rub directly against each other due to minimal joint space. Symptoms are often persistent and can greatly affect daily activities and mobility.
Understanding Your Evaluation
How Is Hip Osteoarthritis Diagnosed?
Hip osteoarthritis is diagnosed through a combination of medical history, physical examination, and imaging studies. These assessments help identify joint degeneration, evaluate the severity of the condition, and exclude other disorders that may produce similar symptoms.
Understanding Your Evaluation
How Is Hip Osteoarthritis Diagnosed?
Hip osteoarthritis is diagnosed through a combination of medical history, physical examination, and imaging studies. These assessments help identify joint degeneration, evaluate the severity of the condition, and exclude other disorders that may produce similar symptoms.
Clinical Evaluation
The doctor reviews the patient’s medical history and examines their hip for pain, stiffness, reduced range of motion, and functional limitations. Movements such as walking, bending, and rotating the hip are assessed.
Imaging Tests
X-rays are typically used to check for joint space narrowing, bone spurs, or cartilage loss. MRI or CT scans may be recommended for more detailed images of the hip joint and surrounding soft tissues.
Laboratory Tests
Rarely used for OA diagnosis but blood tests or analysis of joint fluid may be done to exclude inflammatory arthritis or other conditions that can mimic hip osteoarthritis.
Exploring Treatment Options
Hip Osteoarthritis Treatments in Singapore
Treatment for hip osteoarthritis aims to reduce pain, improve joint mobility, and maintain daily function. Depending on the severity of symptoms and the extent of joint damage, management may involve conservative treatments to relieve symptoms or surgical procedures to restore joint movement.
Non-Surgical Treatment
Non-surgical management focuses on relieving pain, improving joint function, and slowing the progression of hip osteoarthritis without the need for surgery. These approaches include:
Lifestyle Modifications
Making changes such as losing weight and doing low-impact exercises helps reduce stress on the hip joint and maintain mobility.
Medications
Pain relievers and anti-inflammatory drugs help manage discomfort and reduce joint inflammation.
Physiotherapy
Focuses on strengthening muscles around the hip, improving flexibility, and enhancing joint stability to support daily activities.
Assistive Devices
Use of canes, walkers, or orthotics to reduce joint load and improve mobility.
Alternative Therapies
Techniques like acupuncture, massage, or heat/cold therapy can provide additional symptom relief.
Surgical Treatment
Surgery is considered when non-surgical measures are no longer effective in relieving pain or improving joint function. The main surgical options include:
Total Hip Arthroplasty (Hip Replacement)
The damaged joint is replaced with prosthetic components. Highly effective for relieving pain and restoring function in advanced OA.
Hip Resurfacing
The damaged surface of the hip joint is trimmed and covered with a metal cap, preserving more of the patient’s natural bone. It is often recommended for younger, active patients who want to maintain higher activity levels.
Osteotomy
The bone around the hip joint is cut and realigned to redistribute weight and reduce stress on the damaged area. This procedure is typically used for younger patients with structural hip abnormalities.
Arthroscopy
A minimally invasive technique that removes loose fragments, repairs cartilage, or addresses labral tears in the hip joint. It helps improve joint function and can relieve pain with a smaller incision and faster recovery.
Get Relief From Hip Osteoarthritis at HC Orthopaedic Surgery
While there is no cure for hip osteoarthritis, effective management can significantly reduce symptoms and improve one’s quality of life. Early intervention with lifestyle changes, therapy, and medication can slow progression, while surgical options offer lasting relief in advanced stages. Adherence to rehabilitation and ongoing care is crucial for maintaining joint function.

Get Relief From Hip Osteoarthritis at HC Orthopaedic Surgery
While there is no cure for hip osteoarthritis, effective management can significantly reduce symptoms and improve one’s quality of life. Early intervention with lifestyle changes, therapy, and medication can slow progression, while surgical options offer lasting relief in advanced stages. Adherence to rehabilitation and ongoing care is crucial for maintaining joint function.
Our Specialised Team
HC Orthopaedic Surgery, hip fracture care is led by Dr Henry Chan, alongside Dr Nicholas Yeoh, Dr Toon Dong Hao and Dr Tang Zhi Hao. Dr Chan has a special interest in computer-assisted joint replacement surgery and previously spearheaded the Joint Replacement Unit at Tan Tock Seng Hospital, where he performed more than 1,000 joint replacements. In addition, Dr Yeoh completed advanced fellowship training in hip and knee reconstruction at the internationally recognised, high-volume North Sydney Orthopaedic and Sports Medicine Centre, Mater Hospital, Sydney. Together, the team provides comprehensive assessment and tailored treatment to help patients recover safely and return to daily life with confidence.
Frequently Asked Questions (FAQs) About Hip Osteoarthritis
Can hip osteoarthritis get worse over time?
Can hip osteoarthritis cause pain in other areas?
How effective is hip replacement surgery?
Can hip osteoarthritis lead to disability?
Does hip osteoarthritis progress faster in active people?
Can hip osteoarthritis cause a leg to appear shorter?
Meet Our Specialist Team
Our team comprises Dr Henry Chan, Dr Nicholas Yeoh, Dr Toon Dong Hao, and Dr Tang Zhi Hao — experienced orthopaedic surgeons with subspecialty experience and a patient-centred approach to care.

Dr Henry Chan
Medical Director & Senior Consultant Orthopaedic Surgeon
MBBS (S’pore), MRCS (Edinburgh), MMed (Orthopaedic Surgery), FRCS (Edinburgh)
Dr Henry Chan is an experienced orthopaedic surgeon specialising in joint replacement and complex revision surgery. Trained at the renowned Helios Endo-Klinik in Germany under the MOH HMDP scholarship, he has performed over 1,000 joint replacements and specialises in computer-assisted and robotic joint replacement techniques for precise outcomes.

Dr Nicholas Yeoh
Senior Consultant Orthopaedic Surgeon
MBChB (Edinburgh), MRCS (Edinburgh), MMed (Orthopaedic Surgery), FRCS (Edinburgh)
Dr Nicholas Yeoh is an MOH-accredited orthopaedic specialist and Fellow of the Royal College of Surgeons of Edinburgh. Fellowship-trained in hip and knee reconstruction in Sydney under the MOH HMDP scholarship, he specialises in minimally invasive joint replacement, robotic surgery and advanced techniques that enhance recovery and surgical outcomes.

Dr Toon Dong Hao
Senior Consultant Orthopaedic Surgeon
MBChB (Leeds), MRCS (Edinburgh), MMed (Orthopaedic Surgery), FRCS (Edinburgh)
Dr Toon Dong Hao is a skilled orthopaedic surgeon and Fellow of the Royal College of Surgeons of Edinburgh. Fellowship-trained in Advanced Shoulder and Elbow Surgery in Sydney under the MOH HMDP scholarship, Dr Toon specialises in sports injuries, arthroscopic surgery and complex shoulder, elbow and knee procedures to restore function and mobility.

Dr Tang Zhi Hao
Senior Consultant Orthopaedic Surgeon
MBBS (S’pore), MRCS (Edinburgh), MMed (Orthopaedic Surgery), FRCS (Edinburgh)
Dr Tang Zhi Hao is a fellowship-trained orthopaedic surgeon specialising in foot and ankle conditions. He completed his Foot and Ankle Surgery fellowship at Severance Hospital, Yonsei University Health System in Seoul under Professor Jin Woo Lee. Prior to private practice, he served as Consultant and Deputy Head of Orthopaedics at Khoo Teck Puat Hospital.