Plantar Fasciitis (Heel Pain):
Symptoms, Causes and Treatments






Plantar fasciitis is one of the most common causes of heel pain in adults. It often begins with a sharp discomfort under the heel when you take your first steps in the morning or after sitting for a prolonged period. That first step out of bed can feel especially intense. For some, the pain eases after a few minutes of walking, only to return later in the day after long hours on your feet. For others, it becomes a persistent ache that affects walking, exercise and routine activities.
The plantar fascia is a thick band of connective tissue that runs along the bottom of your foot, connecting the heel bone to the toes. It supports the arch of the foot and absorbs shock with every step. When repetitive strain exceeds the tissue’s capacity to recover, small areas of damage can develop, leading to inflammation or degeneration near the heel. Understanding the symptoms, causes and treatment options for plantar fasciitis can help you seek appropriate care early and prevent chronic heel pain from interfering with your daily activities.
What Are the Symptoms of Plantar Fasciitis?
Plantar fasciitis is the most common cause of heel pain, typically presenting with a very specific pattern of discomfort.
Sharp Pain with the First Steps of the Day
The hallmark of plantar fasciitis is intense heel pain in the morning. After a night of rest, the plantar fascia shortens slightly. When you take your first steps, the sudden stretch places tension on the irritated tissue, causing sharp pain that often settles into a dull ache after a few minutes of walking.
Pain After Prolonged Activity or Standing
Although discomfort may ease during light activity, it often worsens after long periods of standing, walking or exercise. Many patients notice increased heel pain at the end of the day rather than during activity itself.
Tenderness at the Bottom of the Heel
Pain is typically localised to the inner underside of the heel, where the plantar fascia attaches to the heel bone. This area may be highly sensitive to pressure, making it uncomfortable to walk barefoot on hard surfaces.
Stiffness in the Foot and Calf
Plantar fasciitis is often associated with tightness in the arch and reduced ankle flexibility, particularly limited dorsiflexion. Tight calf muscles can increase strain on the plantar fascia and contribute to persistent symptoms.
Why It Happens
Common Causes and Risk Factors of Plantar Fasciitis
Plantar fasciitis usually develops due to a combination of repetitive mechanical stress and individual factors that increase strain on the plantar fascia. Rather than a single cause, it is often the result of cumulative overload over time.
Repetitive Impact and Overuse
Activities that involve prolonged walking, running or jumping place repeated tensile load on the plantar fascia. Sudden increases in training intensity or duration can further strain the tissue before it has time to adapt.
Prolonged Standing on Hard Surfaces
Occupations that require long hours on your feet, especially on concrete or tiled floors, create sustained stress at the heel attachment of the fascia.
Abnormal Foot Mechanics
Flat feet, high arches or excessive pronation can alter how weight is distributed across the sole. These changes may increase tension along the plantar fascia with each step.
Tight Calf Muscles or Limited Ankle Mobility
Restricted ankle dorsiflexion increases the pull transmitted from the calf muscles through the heel, raising strain on the plantar fascia during walking and running.
Age
Plantar fasciitis is most common between the ages of 40 and 60, when tissue elasticity gradually declines and recovery from repetitive stress becomes slower.
Excess Body Weight
Carrying excess body weight increases the mechanical load placed on the arch and heel, amplifying strain on the plantar fascia.
Inadequate Footwear
Shoes that lack adequate arch support or cushioning may fail to absorb impact effectively, increasing stress on the heel during daily activities.
Alternative Causes
Other Possible Causes of Heel Pain
Not all heel pain is due to plantar fasciitis. Several other conditions can cause similar symptoms, which is why a proper assessment is important if pain persists or does not follow the typical pattern.
Calcaneal Stress Fracture
A stress fracture of the heel bone can develop after a sudden increase in running or impact activity. Unlike plantar fasciitis, the pain is often more constant, worsens with weight-bearing and may not improve after a few steps.
Achilles Tendinopathy
Pain at the back of the heel, rather than underneath it, may be related to irritation or degeneration of the Achilles tendon. This discomfort is typically aggravated by push-off movements, uphill walking or climbing stairs.
Heel Pad Syndrome
The heel pad acts as a natural cushion. If it becomes thinned or irritated, pain may be felt directly in the centre of the heel, especially when walking on hard surfaces.
Tarsal Tunnel Syndrome
Compression of a nerve along the inside of the ankle can cause burning, tingling or shooting pain into the heel and arch. This differs from the sharp, localised pain typical of plantar fasciitis.
Inflammatory Conditions
Less commonly, systemic conditions such as inflammatory arthritis can cause heel pain, particularly if symptoms occur in both feet or are associated with joint swelling elsewhere.
At HC Orthopaedic Surgery, our foot and ankle specialists provide thorough evaluation to accurately distinguish plantar fasciitis from other causes of heel pain and guide appropriate management.
Understanding Your Evaluation
How Is Plantar Fasciitis Diagnosed?
Plantar fasciitis is usually diagnosed through a detailed medical history and physical examination. Your doctor will ask about the pattern of heel pain, particularly whether it is worse with the first steps in the morning or after periods of rest. A focused examination helps identify localised tenderness and assess foot mechanics, ankle flexibility and calf tightness.
Physical Examination
During the examination, pressure is applied to the underside of the heel, especially near the inner attachment of the plantar fascia. Reproduction of pain in this area is a key clinical sign. Your ankle range of motion, particularly dorsiflexion, may also be assessed, as limited flexibility can increase strain on the fascia. Gait and foot alignment are evaluated to identify contributing mechanical factors.
Ultrasound Imaging
Ultrasound can be used to confirm thickening of the plantar fascia and detect areas of degeneration. It allows real-time assessment and is often sufficient when imaging is required.
X-rays
An X-ray is not routinely necessary for plantar fasciitis but may be performed to rule out other causes of heel pain, such as a calcaneal stress fracture. Heel spurs may be visible, although their presence does not necessarily correlate with symptoms.
MRI Scan
MRI is typically reserved for persistent or atypical cases. It provides detailed evaluation of the plantar fascia and surrounding soft tissues, particularly when symptoms do not improve despite appropriate treatment.
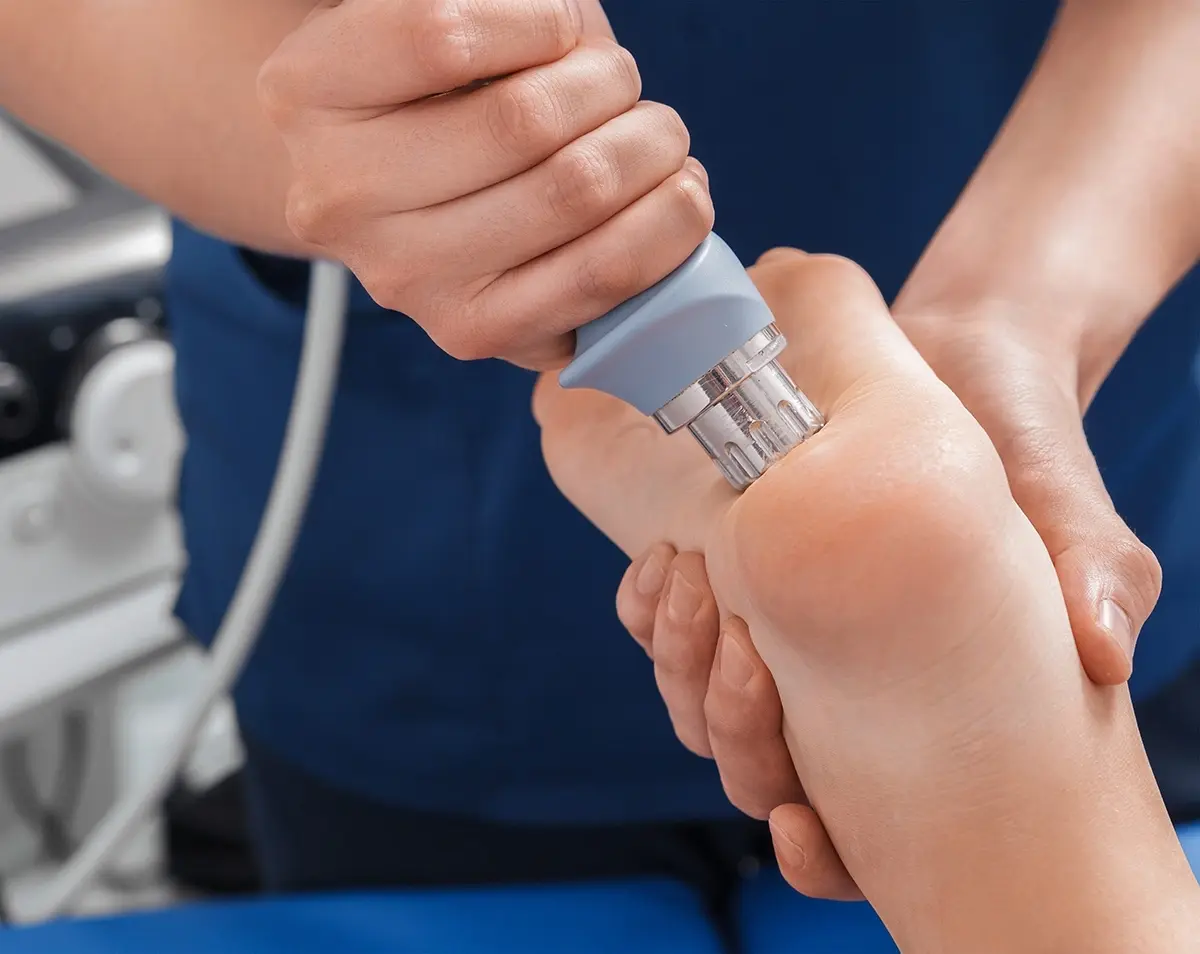
Plantar Fasciitis Treatments in Singapore
Treatment for plantar fasciitis focuses on reducing mechanical strain on the plantar fascia, promoting tissue recovery and correcting contributing biomechanical factors.
Non-Surgical Treatments
Most cases of plantar fasciitis improve without surgery. The goal of non-surgical treatment is to reduce strain on the plantar fascia, relieve pain and address underlying mechanical contributors to prevent recurrence.
Activity Modification
Reducing repetitive impact activities such as running, prolonged standing or jumping allows the fascia time to recover. Low-impact alternatives may be recommended during the healing phase.
Structured Stretching Programme
Targeted stretching of the calf muscles and plantar fascia improves ankle dorsiflexion and reduces tensile load at the heel attachment. Regular, consistent stretching is important for gradual improvement.
Strengthening and Load Management
Progressive strengthening of the intrinsic foot muscles and calf complex improves arch support and load distribution. Controlled loading, rather than prolonged complete rest, supports tissue recovery.
Footwear Optimisation and Orthotics
Supportive footwear with adequate arch support and cushioning helps reduce heel strain. Custom or prefabricated orthotic inserts may redistribute pressure and decrease stress at the fascia attachment.
Night Splints
Night splints maintain the ankle in a gently dorsiflexed position during sleep. This helps reduce morning pain by preventing overnight tightening of the plantar fascia.
Taping Techniques
Temporary taping may provide short-term relief by supporting the arch and offloading the fascia during activity.
Extracorporeal Shockwave Therapy (ESWT)
Shockwave therapy may be considered in chronic cases that do not respond to initial conservative measures. It is thought to stimulate tissue healing in degenerative fascia.
Corticosteroid Injections
Steroid injections may provide short-term pain relief in selected cases. However, they are used cautiously due to the potential risk of plantar fascia rupture or fat pad atrophy and are not considered first-line treatment.
Surgical Treatments
Surgery is considered only when symptoms persist after 6 to 12 months of comprehensive conservative management.
Partial Plantar Fascia Release
This involves releasing a portion of the plantar fascia near its heel attachment to reduce tension. The goal is to relieve pain while preserving arch stability.
Gastrocnemius Recession
In patients with significant calf tightness contributing to limited ankle mobility, surgical lengthening of the gastrocnemius muscle may reduce strain on the plantar fascia.
Heel Spur Removal
Heel spurs are often an incidental finding and are not always the source of pain. Spur removal is only considered if it is clearly contributing to symptoms during surgical intervention.
Rehabilitation and Recovery
Rehabilitation remains essential regardless of treatment approach. Gradual return to activity, guided by strength and flexibility milestones, helps reduce recurrence. Most patients improve within several months when mechanical contributors are addressed appropriately.
Find Relief From Heel Pain at HC Orthopaedic Surgery
Plantar fasciitis can range from a mild, activity-related irritation to persistent heel pain that limits daily movement. Because several conditions can mimic its symptoms, accurate diagnosis and a structured treatment plan are essential. Early, targeted management helps reduce ongoing strain on the plantar fascia, prevent chronic degeneration and support a steady return to normal activity.

Find Relief From Heel Pain at HC Orthopaedic Surgery
Plantar fasciitis can range from a mild, activity-related irritation to persistent heel pain that limits daily movement. Because several conditions can mimic its symptoms, accurate diagnosis and a structured treatment plan are essential. Early, targeted management helps reduce ongoing strain on the plantar fascia, prevent chronic degeneration and support a steady return to normal activity.
Our Specialised Team
At HC Orthopaedic Surgery, our foot and ankle specialists provide comprehensive evaluation and evidence-based treatment for plantar fasciitis and other causes of heel pain. The practice is led by Dr Henry Chan, together with Dr Nicholas Yeoh, Dr Toon Dong Hao and Dr Tang Zhi Hao, whose clinical interests include foot and ankle surgery, sports injuries, and fractures and trauma. We focus on relieving pain, correcting underlying mechanical factors and restoring long-term foot function. Schedule an appointment for a personalised assessment and treatment plan.
Frequently Asked Questions (FAQs) About Plantar Fasciitis
Is a heel spur the same as plantar fasciitis?
Can I continue to run with plantar fasciitis?
Why does it hurt more after I sit down for a while?
How long does it take for plantar fasciitis to heal?
Are flip-flops bad for plantar fasciitis?
Meet Our Specialist Team
Our team comprises Dr Henry Chan, Dr Nicholas Yeoh, Dr Toon Dong Hao, and Dr Tang Zhi Hao — experienced orthopaedic surgeons with subspecialty experience and a patient-centred approach to care.

Dr Henry Chan
Medical Director & Senior Consultant Orthopaedic Surgeon
MBBS (S’pore), MRCS (Edinburgh), MMed (Orthopaedic Surgery), FRCS (Edinburgh)
Dr Henry Chan is an experienced orthopaedic surgeon specialising in joint replacement and complex revision surgery. Trained at the renowned Helios Endo-Klinik in Germany under the MOH HMDP scholarship, he has performed over 1,000 joint replacements and specialises in computer-assisted and robotic joint replacement techniques for precise outcomes.

Dr Nicholas Yeoh
Senior Consultant Orthopaedic Surgeon
MBChB (Edinburgh), MRCS (Edinburgh), MMed (Orthopaedic Surgery), FRCS (Edinburgh)
Dr Nicholas Yeoh is an MOH-accredited orthopaedic specialist and Fellow of the Royal College of Surgeons of Edinburgh. Fellowship-trained in hip and knee reconstruction in Sydney under the MOH HMDP scholarship, he specialises in minimally invasive joint replacement, robotic surgery and advanced techniques that enhance recovery and surgical outcomes.

Dr Toon Dong Hao
Senior Consultant Orthopaedic Surgeon
MBChB (Leeds), MRCS (Edinburgh), MMed (Orthopaedic Surgery), FRCS (Edinburgh)
Dr Toon Dong Hao is a skilled orthopaedic surgeon and Fellow of the Royal College of Surgeons of Edinburgh. Fellowship-trained in Advanced Shoulder and Elbow Surgery in Sydney under the MOH HMDP scholarship, Dr Toon specialises in sports injuries, arthroscopic surgery and complex shoulder, elbow and knee procedures to restore function and mobility.

Dr Tang Zhi Hao
Senior Consultant Orthopaedic Surgeon
MBBS (S’pore), MRCS (Edinburgh), MMed (Orthopaedic Surgery), FRCS (Edinburgh)
Dr Tang Zhi Hao is a fellowship-trained orthopaedic surgeon specialising in foot and ankle conditions. He completed his Foot and Ankle Surgery fellowship at Severance Hospital, Yonsei University Health System in Seoul under Professor Jin Woo Lee. Prior to private practice, he served as Consultant and Deputy Head of Orthopaedics at Khoo Teck Puat Hospital.