Flat Feet:
Symptoms, Causes and Treatments in Singapore






Flat feet are a common condition where the arches of the feet appear low or absent when standing. Some people have flat feet without pain, while others experience discomfort in the feet, ankles or even the knees after prolonged walking or standing. You may notice your shoes wearing out unevenly, your feet feeling tired more quickly, or difficulty finding supportive footwear.
Flat feet, medically known as pes planus, occur when the arch of the foot collapses or does not fully develop. This changes how weight is distributed across the foot and can alter overall walking mechanics. While many cases are mild and require no treatment, symptomatic flat feet may benefit from targeted management to reduce strain and improve alignment.
What Are the Signs and Symptoms of Flat Feet?
Flat feet can present differently depending on whether the condition is flexible or rigid, and whether it is causing strain on surrounding structures. Some individuals have no symptoms, while others develop pain or fatigue with activity. Common signs and symptoms of flat feet include:
Flat or Low Arches
The arch appears reduced or flattened when standing, and more of the sole may contact the ground. In flexible flat feet, the arch may reappear when sitting or standing on tiptoe.
Foot Pain
Discomfort may develop in the arch, heel or inner ankle due to increased strain on supporting muscles, ligaments and tendons.
Swelling Along the Inner Ankle
Tenderness or swelling may occur along the inside of the ankle if the posterior tibial tendon is under strain.
Difficulty Standing or Walking
Prolonged standing or walking may become uncomfortable due to altered load distribution across the foot.
Uneven Shoe Wear
Shoes may wear out more quickly on the inner side, reflecting changes in weight distribution and gait.
Foot Fatigue
The muscles supporting the arch may tire more easily, particularly after extended activity.
Changes in Gait
Flat feet can alter walking mechanics, which may contribute to discomfort in the ankles, knees or hips over time.
If you suspect you have flat feet or are experiencing persistent foot pain, seek assessment from the foot and ankle specialists at HC Orthopaedic Surgery for an accurate diagnosis and appropriate management.
Why It Happens
Causes and Risk Factors for Flat Feet
Flat feet can be present from childhood or develop later in life. In many cases, the condition results from a combination of inherited foot structure and factors that place prolonged strain on the arch-supporting tissues.
Inherited Foot Structure
Some people are born with more flexible ligaments or foot shapes that predispose them to low arches. In children and adolescents, flexible flat feet are common and often painless.
Posterior Tibial Tendon Dysfunction
In adults, one of the most important causes of progressive flat feet is weakening or degeneration of the posterior tibial tendon. This tendon helps support the arch, and when it becomes strained or torn, the arch may gradually collapse.
Age-related Changes
As we age, tendons and ligaments lose elasticity and strength. Over time, cumulative mechanical stress can contribute to arch flattening.
Injury or Trauma
Fractures, ligament injuries or damage to the posterior tibial tendon can alter foot alignment and lead to acquired flatfoot deformity.
Obesity
Excess body weight increases the load transmitted through the arch with every step, placing additional strain on supporting structures.
Inflammatory or Neuromuscular Conditions
Conditions such as rheumatoid arthritis, diabetes-related tendon changes or certain neuromuscular disorders can affect joint stability and contribute to arch collapse.

Understanding the Differences
What Are the Types of Flat Feet?
Flat feet can be classified based on flexibility and underlying cause.
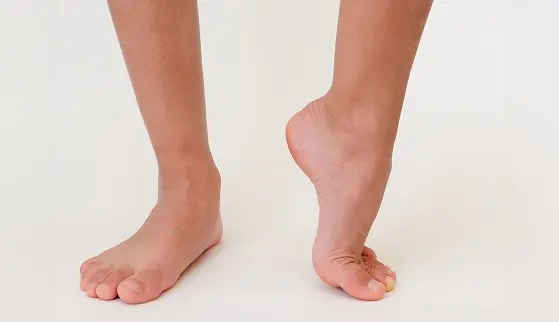
Flexible Flat Feet
This is the most common type. The arch is visible when the foot is lifted or when standing on tiptoe, but flattens when bearing weight. Flexible flat feet are common in children and many adults, and may not cause symptoms unless strain develops over time.

Rigid Flat Feet
In rigid flat feet, the arch remains absent whether sitting or standing. The foot may feel stiff, and movement at certain joints can be limited. This type is more likely to cause discomfort and may be associated with structural bone abnormalities.
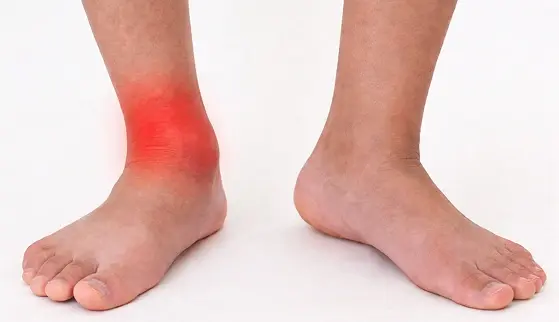
Acquired Flat Feet
This develops later in life, often due to weakening of the posterior tibial tendon, which supports the arch. The condition may begin with pain and swelling along the inner ankle before progressing to visible arch collapse and heel tilting outward. Without treatment, it can gradually worsen and affect walking mechanics.
Understanding Your Evaluation
How Are Flat Feet Diagnosed?
Diagnosis begins with a detailed medical history and physical examination to assess symptoms, arch appearance and overall foot alignment. The goal is to determine whether the flat feet are flexible or rigid, whether they are symptomatic, and whether there is tendon or joint involvement.
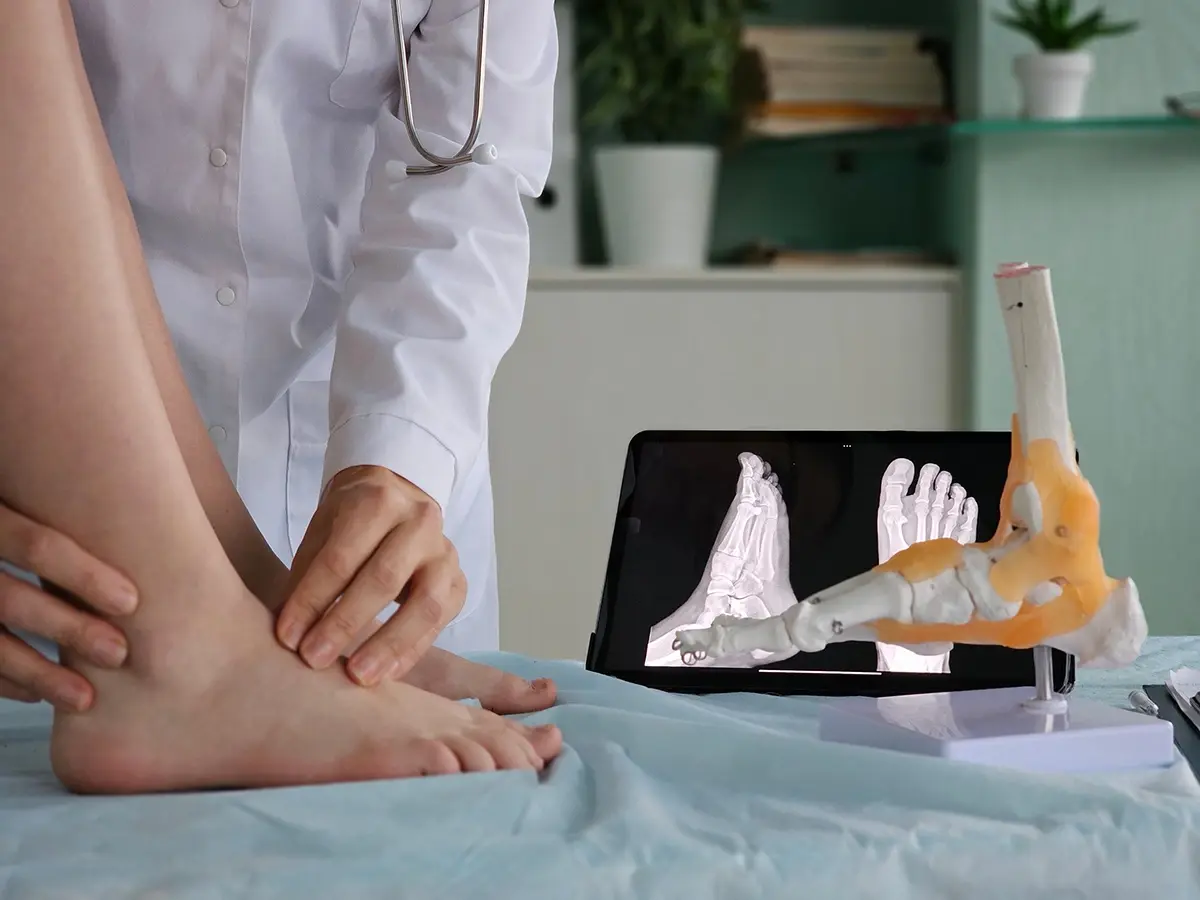
Functional Testing
You may be asked to stand on tiptoe or perform a single-leg heel raise. These tests assess arch flexibility and the function of the posterior tibial tendon, which plays a key role in maintaining arch support.
Gait Assessment
Your walking pattern is observed to identify excessive inward rolling of the foot, heel tilting or compensatory movements that may contribute to ankle, knee or hip discomfort.
Weight-Bearing X-rays
Standing X-rays are often performed when symptoms are present or progressive. Because flat feet are load-dependent deformities, imaging under weight-bearing conditions allows accurate assessment of bone alignment and severity.
Ultrasound or MRI
If posterior tibial tendon dysfunction, ligament injury or arthritis is suspected, advanced imaging may be recommended to evaluate soft tissue structures in greater detail.
Flat Feet Treatments in Singapore
Treatment for flat feet depends on whether the condition is painful, progressive or affecting walking mechanics. Many people with flat feet do not require treatment. Management is recommended when symptoms develop, when there is tendon dysfunction, or when the deformity progresses over time.
Non-Surgical Treatment
For most patients, treatment begins conservatively. The aim is to reduce strain on the arch, support tendon function and improve overall foot alignment.
Footwear Modification
Supportive shoes with structured arch support and a firm heel counter can improve stability and reduce excessive inward rolling of the foot.
Orthotic Insoles
Custom or prefabricated orthotics may help redistribute pressure, support the arch and reduce stress on the posterior tibial tendon.
Physiotherapy and Strengthening
Targeted exercises focus on strengthening the muscles that support the arch, particularly the posterior tibial muscle. Calf stretching may also improve ankle flexibility and reduce strain.
Activity Modification
Reducing high-impact activities during painful phases allows inflamed tendons and soft tissues to recover.
Pain Management
Short-term use of anti-inflammatory medication or ice may help manage flare-ups in symptomatic cases.
Surgical Treatment
Flat foot correction surgery is considered when flat feet cause persistent pain, progressive deformity or tendon dysfunction that does not improve with appropriate non-surgical treatment. Most individuals respond well to conservative measures, so surgery is typically reserved for more advanced or symptomatic cases. The type of procedure depends on the severity of the deformity, tendon integrity and joint involvement. The goal is to restore alignment, improve stability and relieve pain while preserving as much natural foot function as possible.
Potential Long Term Effects
Complications That Can Develop from Flat Feet
While many people with flat feet remain symptom-free, altered foot mechanics can place strain on surrounding structures and lead to secondary problems over time.

Potential Long Term Effects
Complications That Can Develop from Flat Feet
While many people with flat feet remain symptom-free, altered foot mechanics can place strain on surrounding structures and lead to secondary problems over time.
Accessory Navicular Syndrome
Some individuals have an extra bone on the inner side of the foot called an accessory navicular. In flat feet, increased strain on the posterior tibial tendon can irritate this area, causing pain and swelling along the inner midfoot.
Posterior Tibial Tendon Dysfunction
Chronic overload of the tendon that supports the arch may lead to weakening or degeneration. This can result in progressive arch collapse and worsening deformity.
Joint Strain and Arthritis
Abnormal load distribution may increase stress across the midfoot and hindfoot joints, potentially contributing to stiffness or degenerative changes in long-standing cases.
Supporting Long-term Foot Stability at HC Orthopaedic Surgery
Flat feet can range from a painless structural variation to a progressive condition that affects walking mechanics and overall lower-limb alignment. While many individuals do not require treatment, persistent pain, tendon strain or visible arch collapse should not be ignored. Early evaluation allows for appropriate management, whether through footwear modification, orthotic support or more structured intervention in advanced cases.

Supporting Long-term Foot Stability at HC Orthopaedic Surgery
Flat feet can range from a painless structural variation to a progressive condition that affects walking mechanics and overall lower-limb alignment. While many individuals do not require treatment, persistent pain, tendon strain or visible arch collapse should not be ignored. Early evaluation allows for appropriate management, whether through footwear modification, orthotic support or more structured intervention in advanced cases.
Our Specialised Team
At HC Orthopaedic Surgery, our foot and ankle specialists provide comprehensive assessment and tailored treatment for both flexible and adult-acquired flatfoot. The practice is led by Dr Henry Chan, together with Dr Nicholas Yeoh, Dr Toon Dong Hao and Dr Tang Zhi Hao, whose clinical interests include foot and ankle surgery, sports injuries, and fractures and trauma. Our focus is on preserving foot function, restoring alignment where necessary and supporting durable, long-term mobility.
Frequently Asked Questions (FAQs) About Flat Feet
Can flat feet cause pain in other parts of the body?
Are flat feet always painful?
When is surgery necessary for flat feet?
Are both feet always affected by flat feet?
Can losing weight help reduce flat foot pain?
Meet Our Specialist Team
Our team comprises Dr Henry Chan, Dr Nicholas Yeoh, Dr Toon Dong Hao, and Dr Tang Zhi Hao — experienced orthopaedic surgeons with subspecialty experience and a patient-centred approach to care.

Dr Henry Chan
Medical Director & Senior Consultant Orthopaedic Surgeon
MBBS (S’pore), MRCS (Edinburgh), MMed (Orthopaedic Surgery), FRCS (Edinburgh)
Dr Henry Chan is an experienced orthopaedic surgeon specialising in joint replacement and complex revision surgery. Trained at the renowned Helios Endo-Klinik in Germany under the MOH HMDP scholarship, he has performed over 1,000 joint replacements and specialises in computer-assisted and robotic joint replacement techniques for precise outcomes.

Dr Nicholas Yeoh
Senior Consultant Orthopaedic Surgeon
MBChB (Edinburgh), MRCS (Edinburgh), MMed (Orthopaedic Surgery), FRCS (Edinburgh)
Dr Nicholas Yeoh is an MOH-accredited orthopaedic specialist and Fellow of the Royal College of Surgeons of Edinburgh. Fellowship-trained in hip and knee reconstruction in Sydney under the MOH HMDP scholarship, he specialises in minimally invasive joint replacement, robotic surgery and advanced techniques that enhance recovery and surgical outcomes.

Dr Toon Dong Hao
Senior Consultant Orthopaedic Surgeon
MBChB (Leeds), MRCS (Edinburgh), MMed (Orthopaedic Surgery), FRCS (Edinburgh)
Dr Toon Dong Hao is a skilled orthopaedic surgeon and Fellow of the Royal College of Surgeons of Edinburgh. Fellowship-trained in Advanced Shoulder and Elbow Surgery in Sydney under the MOH HMDP scholarship, Dr Toon specialises in sports injuries, arthroscopic surgery and complex shoulder, elbow and knee procedures to restore function and mobility.

Dr Tang Zhi Hao
Senior Consultant Orthopaedic Surgeon
MBBS (S’pore), MRCS (Edinburgh), MMed (Orthopaedic Surgery), FRCS (Edinburgh)
Dr Tang Zhi Hao is a fellowship-trained orthopaedic surgeon specialising in foot and ankle conditions. He completed his Foot and Ankle Surgery fellowship at Severance Hospital, Yonsei University Health System in Seoul under Professor Jin Woo Lee. Prior to private practice, he served as Consultant and Deputy Head of Orthopaedics at Khoo Teck Puat Hospital.