Cartilage Repair
in Singapore






Joint pain that does not seem to improve can slowly start to affect everyday life. Simple movements such as climbing stairs, exercising or even walking for longer periods may become uncomfortable. In some cases, this may be linked to cartilage damage in the knee, hip or other joints. Because cartilage acts as a smooth, protective layer that allows joints to move easily and absorb impact, damage to it can lead to ongoing pain, swelling or stiffness.
When these symptoms persist or begin to limit normal activities, treatments that address the damaged cartilage may be considered. Cartilage repair aims to restore or regenerate the affected cartilage so the joint can move more smoothly and with less discomfort. As orthopaedic techniques continue to advance, several cartilage repair approaches are now available to help manage joint damage while preserving the natural joint. For suitable patients, these treatments may help relieve symptoms, improve joint function and support a return to daily activities.
Conditions Treated
What Is Cartilage Repair and Who Needs it?
Cartilage repair refers to procedures that aim to restore damaged cartilage within a joint. Instead of simply managing symptoms, these treatments focus on repairing the affected area or encouraging the body to regenerate new cartilage tissue. The goal is to improve joint function while preserving the natural joint structure.
Because cartilage injuries can vary in size, depth and location, treatment is usually tailored to the individual. An orthopaedic specialist will typically assess the joint using physical examination and imaging, such as MRI, to determine whether cartilage repair may be appropriate and which technique may be most suitable.
Cartilage repair may be recommended for individuals who meet certain clinical criteria, such as:
- Individuals with localised cartilage injuries caused by sports injuries or trauma
- Patients who experience persistent joint pain, swelling or catching during movement
- Younger or active individuals with cartilage damage but without advanced arthritis
- People with focal cartilage defects identified through imaging such as MRI
- Patients who want to preserve their natural joint and delay more extensive procedures such as joint replacement
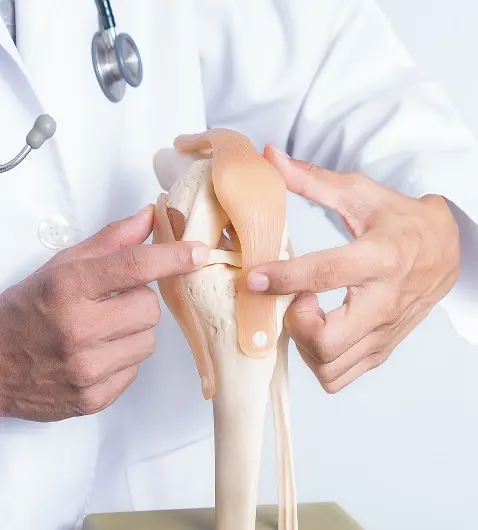
Types of Cartilage Repair Treatments in Singapore
Several cartilage repair procedures are available today, each designed to address different types of cartilage damage within the joint.
Microfracture/Nanofracture
Microfracture and nanofracture are commonly used minimally invasive techniques for treating small, localised cartilage defects. During the procedure, the surgeon creates tiny holes in the subchondral bone beneath the damaged cartilage. This allows bone marrow cells to enter the defect and form new cartilage-like tissue that helps cover the exposed area.
The goal of the procedure is to stimulate the formation of fibrocartilage, which can provide a protective surface over the damaged region and help reduce symptoms. However, fibrocartilage is not identical to the original hyaline cartilage found in healthy joints and may be less durable over time. For this reason, the procedure is generally considered for smaller cartilage defects, particularly in younger patients.
Osteochondral Autograft Transfer (OATS)
Osteochondral Autograft Transfer, also known as OATS, involves transplanting healthy cartilage and the underlying bone from another part of the patient’s joint. The graft is usually taken from a non-weight-bearing area and placed into the damaged site to restore the joint surface.
Because the transplanted tissue contains natural hyaline cartilage, the goal is to reconstruct the defect with cartilage that closely resembles the original joint surface. This technique is often considered for small to moderate cartilage defects where healthy donor tissue can be safely harvested. However, the amount of cartilage that can be taken from the patient’s own joint is limited, which may restrict its use for larger defects.
Osteochondral Allograft Transplantation
Osteochondral allograft transplantation is typically used for larger or more complex cartilage injuries. Instead of using tissue from the patient’s own joint, this procedure uses cartilage and bone from a donor graft. The graft is shaped to fit the damaged area and implanted to restore the joint surface.
The goal is to replace extensive cartilage damage with mature cartilage that can help improve joint function and reduce symptoms. This approach can be useful when the defect is too large for autograft techniques. However, the availability of suitable donor tissue may be limited, and there is a small risk of immune response or graft-related complications.
Autologous Matrix Induced Chondrogenesis (AMIC)
Autologous Matrix-Induced Chondrogenesis (AMIC) is a cartilage repair technique that builds on the principles of microfracture. After the surgeon prepares the cartilage defect and performs microfracture or nanofracture to release bone marrow cells, a bioresorbable collagen scaffold is placed over the treated area.
This scaffold helps stabilise the clot formed by the bone marrow cells and provides a structure that supports cell attachment and growth. The aim is to encourage the formation of cartilage-like tissue that may resemble hyaline cartilage more closely than microfracture alone. AMIC is often considered for medium-sized cartilage defects, particularly in younger and more active individuals.
Arthroscopic Debridement and Lavage
Arthroscopic debridement and lavage is a minimally invasive procedure that focuses on improving joint symptoms rather than regenerating cartilage. During the procedure, the surgeon removes loose cartilage fragments, smooths rough cartilage surfaces and flushes the joint with fluid.
The goal is to reduce mechanical irritation within the joint, which may help relieve symptoms such as catching, locking or discomfort during movement. This procedure is sometimes considered for early-stage cartilage damage or when other cartilage repair techniques are not suitable. However, it does not restore damaged cartilage and is generally associated with short-term symptom relief rather than long-term regeneration.
Treatment Considerations
Factors Influencing the Choice of Cartilage Repair
The most suitable cartilage repair technique depends on several clinical considerations. Orthopaedic specialists evaluate the joint carefully before recommending a specific procedure.
Treatment Considerations
Factors Influencing the Choice of Cartilage Repair
The most suitable cartilage repair technique depends on several clinical considerations. Orthopaedic specialists evaluate the joint carefully before recommending a specific procedure.
- Patient Factors
Age, activity level and overall health can influence which repair method is appropriate. For example, younger and more active patients may benefit from joint-preserving procedures that aim to restore cartilage function.
- Characteristics of the Cartilage Defect
The size, depth and location of the cartilage injury play an important role in determining the treatment approach. Some procedures are better suited for small, localised defects, while others are designed to address larger areas of damage.
- Surgical Considerations
The complexity of the procedure, the surgeon’s expertise and the availability of specialised techniques or graft materials may also influence the treatment plan.
What to Expect From Cartilage Repair
How to Prepare
- Adjust or stop certain medications as instructed by the surgeon
- Undergo pre-operative tests such as blood tests or cardiac assessment
- Arrange for home support during the early recovery period
- Prepare mobility aids such as crutches or walkers if recommended
- Set up a safe recovery space at home with essentials within easy reach
Procedure Overview
Aftercare and Recovery
- Follow the surgeon’s instructions on weight-bearing and activity restrictions
- Attend recommended physiotherapy sessions to rebuild strength and flexibility
- Keep the joint elevated when possible to help reduce swelling
- Apply ice or cold therapy as advised to manage pain and inflammation
- Maintain a balanced diet and stay well-hydrated to support tissue healing
- Avoid high-impact activities until cleared by the doctor
- Monitor the surgical site for signs of infection and report any concerns promptly
Treatment Benefits
How Cartilage Repair Helps Restore Joint Function
Depending on the severity and location of the cartilage injury, cartilage repair may help to:
Reduce joint pain
by addressing damaged cartilage that causes irritation and inflammation
Improve mobility and flexibility
by restoring a smoother joint surface for movement
Support joint stability
by improving how the joint distributes weight and pressure
Slow further joint degeneration
by protecting underlying bone from continued wear
Delay or prevent more invasive procedures
such as joint replacement in suitable patients
With appropriate surgical techniques and rehabilitation, cartilage repair can help patients return to daily activities and maintain better joint function over time.
Understanding the Risks
Potential Risks and Complications of Cartilage Repair
Cartilage repair procedures are generally safe when performed by an experienced orthopaedic surgeon. However, as with any surgical procedure, there are potential risks and complications that patients should be aware of. Understanding these risks helps patients make informed decisions and recognise when to seek medical advice during recovery.
Possible risks and complications may include:
Infection
at the surgical site, which may require antibiotics or additional treatment
Bleeding or swelling
around the joint after surgery
Blood clots
particularly in the lower limbs after knee procedures
Stiffness or reduced range of motion
during the recovery period
Persistent pain
if the cartilage does not heal as expected
Failure of the cartilage repair
which may require further treatment or revision surgery
Careful surgical technique, proper rehabilitation, and adherence to post-operative instructions help reduce the likelihood of complications and support optimal recovery. Patients should contact their doctor if they experience severe pain, increasing swelling, fever, or other concerning symptoms after surgery.
Cost of Cartilage Repair in Singapore
The cost of cartilage repair in Singapore can vary based on the individual patient’s condition and the surgical approach required.
Key Cost Drivers
Several factors can affect the total cost of cartilage repair surgery, including:
Type of cartilage repair technique used
Size and location of the cartilage defect
Hospital or surgical facility fees
Use of specialised implants, grafts, or biologic materials
Post-surgical rehabilitation

Insurance and Financing
Many cartilage repair procedures may be claimable under Integrated Shield Plans and private insurance, depending on the patient’s coverage and the medical necessity of the procedure. Patients may also be able to use MediSave for approved surgical treatments.
At HC Orthopaedic Surgery, our team can help review your insurance coverage and provide clear cost estimates so you can better plan for treatment.
Restoring Joint Health with HC Orthopaedic Surgery
Cartilage damage can affect how a joint moves, feels and functions over time. With appropriate evaluation and treatment, cartilage repair procedures may help restore smoother joint movement, relieve discomfort and support a more active lifestyle. Because cartilage injuries vary widely in their cause, size and location, selecting the right treatment approach requires careful assessment and a personalised care plan that focuses on long-term joint health and function.

Restoring Joint Health with HC Orthopaedic Surgery
Cartilage damage can affect how a joint moves, feels and functions over time. With appropriate evaluation and treatment, cartilage repair procedures may help restore smoother joint movement, relieve discomfort and support a more active lifestyle. Because cartilage injuries vary widely in their cause, size and location, selecting the right treatment approach requires careful assessment and a personalised care plan that focuses on long-term joint health and function.
Our Specialised Team
At HC Orthopaedic Surgery, patients receive comprehensive evaluation and cartilage repair treatment tailored to their specific condition and activity needs. Our orthopaedic team, including Dr Henry Chan, Dr Nicholas Yeoh, Dr Toon Dong Hao and Dr Tang Zhi Hao, provides evidence-based care using modern joint-preserving techniques and structured rehabilitation to support optimal recovery. Schedule an appointment with HC Orthopaedic Surgery to discuss your symptoms and explore suitable cartilage repair options.
Frequently Asked Questions (FAQs) About Cartilage Repair
What joints can be treated with cartilage repair?
Who is a suitable candidate for cartilage repair?
Will I be able to exercise again after cartilage repair?
How long does recovery from cartilage repair take?
Will I experience pain after cartilage repair surgery?
How long does the repaired cartilage last?
Can cartilage repair be done at the same time as other knee surgeries?
How is cartilage repair different from joint replacement?
What lifestyle habits help support cartilage healing?
Meet Our Specialist Team
Our team comprises Dr Henry Chan, Dr Nicholas Yeoh, Dr Toon Dong Hao, and Dr Tang Zhi Hao — experienced orthopaedic surgeons with subspecialty experience and a patient-centred approach to care.

Dr Henry Chan
Medical Director & Senior Consultant Orthopaedic Surgeon
MBBS (S’pore), MRCS (Edinburgh), MMed (Orthopaedic Surgery), FRCS (Edinburgh)
Dr Henry Chan is an experienced orthopaedic surgeon specialising in joint replacement and complex revision surgery. Trained at the renowned Helios Endo-Klinik in Germany under the MOH HMDP scholarship, he has performed over 1,000 joint replacements and specialises in computer-assisted and robotic joint replacement techniques for precise outcomes.

Dr Nicholas Yeoh
Senior Consultant Orthopaedic Surgeon
MBChB (Edinburgh), MRCS (Edinburgh), MMed (Orthopaedic Surgery), FRCS (Edinburgh)
Dr Nicholas Yeoh is an MOH-accredited orthopaedic specialist and Fellow of the Royal College of Surgeons of Edinburgh. Fellowship-trained in hip and knee reconstruction in Sydney under the MOH HMDP scholarship, he specialises in minimally invasive joint replacement, robotic surgery and advanced techniques that enhance recovery and surgical outcomes.

Dr Toon Dong Hao
Senior Consultant Orthopaedic Surgeon
MBChB (Leeds), MRCS (Edinburgh), MMed (Orthopaedic Surgery), FRCS (Edinburgh)
Dr Toon Dong Hao is a skilled orthopaedic surgeon and Fellow of the Royal College of Surgeons of Edinburgh. Fellowship-trained in Advanced Shoulder and Elbow Surgery in Sydney under the MOH HMDP scholarship, Dr Toon specialises in sports injuries, arthroscopic surgery and complex shoulder, elbow and knee procedures to restore function and mobility.

Dr Tang Zhi Hao
Senior Consultant Orthopaedic Surgeon
MBBS (S’pore), MRCS (Edinburgh), MMed (Orthopaedic Surgery), FRCS (Edinburgh)
Dr Tang Zhi Hao is a fellowship-trained orthopaedic surgeon specialising in foot and ankle conditions. He completed his Foot and Ankle Surgery fellowship at Severance Hospital, Yonsei University Health System in Seoul under Professor Jin Woo Lee. Prior to private practice, he served as Consultant and Deputy Head of Orthopaedics at Khoo Teck Puat Hospital.